Researchers to test 'breakthrough' pediatric leukemia treatment
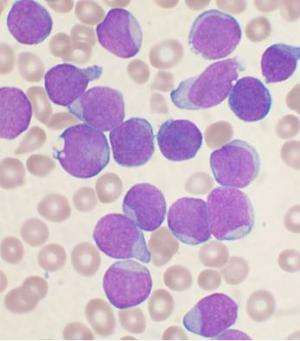
A promising method of immunotherapy to treat children with relapsed acute lymphocytic leukemia (ALL) is opening at the University of Wisconsin Carbone Cancer Center and American Family Children's Hospital. The trial is open to relapsed/refractory pediatric ALL patients who have limited treatment options.
The UW Carbone Cancer Center is among several centers participating in a multi-site trial to test this immunotherapy, named CTL019, which was developed by a research team at the University of Pennsylvania. Initial clinical trials of CTL019 have taken place at both Penn and The Children's Hospital of Philadelphia. Penn and Novartis have an exclusive global collaboration to research, develop and commercialize targeted chimeric antigen receptor (CAR) immunotherapies for the treatment of cancers. The therapy received the Food and Drug Administration's Breakthrough Therapy designation on July 7, 2014.
This experimental therapy for ALL uses a CAR to attach to, and hunt, leukemia cells expressing a CD19 antigen by using the study participants' T-cells.
In this experimental treatment, T-cells are reprogrammed to express the CAR receptor, which may detect the leukemia and potentially destroy the cells.
The process begins by extracting T-cells from the study participants. The cells are sent to a lab for reprogramming. "Once the T-cells are reprogrammed, the modified cells are shipped back with the special cells," says Christian Capitini, the UW pediatric hematology oncologist who is principal investigator of the clinical trial.
Both the collection of T-cells and the infusion can be outpatient procedures.
Capitini says patients can potentially develop symptoms of cytokine release syndrome. Cytokines are inflammatory molecules that are released when there is inflammation. The CAR cells grow in massive numbers while in the patient and trigger the release of cytokines.
"Symptoms include high fevers, chills and headaches, but some very serious symptoms, like dangerous blood pressure drops or breathing difficulties, may develop," says Capitini.
Patients must stay close to the hospital because of these potentially rapidly developing symptoms.
"At this point, the patients are hospitalized and some may be admitted to the intensive care unit if necessary," says Capitini. "Patients are treated with an anti-inflammatory drug used for rheumatoid arthritis called tocilizumab. The symptoms may resolve in a matter of hours after administration of the drug."
The follow-up care may involve a monthly immunoglobulin infusion because all normal B-cells are killed by the therapy.
More information: Those interested in joining the trial should check with their physician or refer to the clinical site to determine eligibility: clinicaltrials.gov/ct2/show/st … l019&rank=1#contacts