Sieve-like structure regulates the transport of proteins and migration of white blood cells into lymph nodes
Researchers have uncovered a sieve-like structure in lymph nodes that regulates the transport of proteins and migration of white blood cells into lymph nodes. The discovery, made by scientists working at the University of Turku, Finland, will provide new insights into rapid defence responses in the human immune system. The research was carried out with funding from the Academy of Finland and the Sigrid Juselius Foundation.
The researchers found that the plasmalemma vesicle-associated protein (PLVAP), often used as a marker for blood vessels, is expressed in lymph nodes not only in the blood vessels but also in the lymphatic vessels that transport tissue fluids. "This was a surprising result. For nearly 30 years, the PLVAP protein has been regarded as the best marker protein for blood vessels in pathology and biomedical research. Yet, no one has ever reported having found PLVAP in lymphatic vessels. The most likely explanation is that the protein only appears in the lymphatic vessels underneath the lymph node capsule, not in dermal lymphatic vessels or anywhere else in the lymphatic system," says Senior Researcher Kaisa Auvinen, PhD, who was in charge of bioimaging in the study.
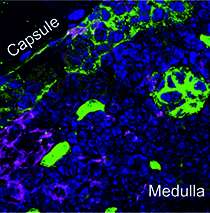
The team used light and electron microscopy to show that lymphatic endothelial cells, which line the interior surface of the lymph node capsule, contain a number of channels that penetrate the whole thickness of the cells. The PLVAP protein seems to form a sieve-like structure that partly closes the openings of these transendothelial channels. When the researchers deleted the PLVAP protein from the endothelial cells, the channels remained fully open.
Analyses of the imaging data led the team to study how the lack of the PLVAP protein would affect the inflammatory response. They administered a foreign protein subcutaneously and found that the foreign protein was transported to the cells residing inside the lymph node much more quickly when the lymphatic vessels lacked the PLVAP protein. In the absence of the PLVAP protein, also large molecules, which the PLVAP sieve normally blocks from entering the node, were able to stimulate the cells of the body's defence system. White blood cells, which enter the lymph node via the lymphatic vessels, also migrated deep into the node much more effectively if the PLVAP sieve was missing.
A new way to fight severe inflammation?
"The common kitchen sink is a good analogy. The strainer at the bottom of the sink filters out excess debris. If you were to remove the strainer completely, it would allow even larger debris into the drain. In lymph nodes, the PLVAP protein is like the metal sieve of a strainer, perforated with tiny holes," explains Senior Researcher Pia Rantakari, PhD, one of the key investigators behind the research.
The team's findings explain how a foreign material stuck under the skin is transported and filtered in a matter of minutes to the interior parts of the draining lymph node. Once in the node, the material comes into contact with the immune cells that automatically initiate the inflammatory response and thereby triggers the body's defence systems.
"This reaction is most commonly seen in the form of swollen lymph nodes caused by flu or vaccination. Since we were able to regulate the function of the PLVAP sieve using antibodies, our findings may also offer potential for restraining inappropriately strong inflammatory responses in certain inflammatory and infectious diseases," say Auvinen and Rantakari.
More information: "The endothelial protein PLVAP in lymphatics controls the entry of lymphocytes and antigens into lymph nodes." Nature Immunology (2015) DOI: 10.1038/ni.3101













