Cancer drug shows promise as cure for hepatitis B

Australian scientists have found a potential cure for hepatitis B virus (HBV) infections, with a promising new treatment proving 100 per cent successful in eliminating the infection in preclinical models.
Australian patients are now the first in the world to have access to the potential treatment - a combination of an antiviral drug and an anti-cancer drug - which is in phase 1/2a clinical trials in Melbourne, Perth and Adelaide.
Scientists from Melbourne's Walter and Eliza Hall Institute developed the combination treatment using birinapant, a drug developed by US biotech company TetraLogic Pharmaceuticals for treating cancer. Hepatitis B is a chronic viral disease that is currently incurable.
Dr Marc Pellegrini, Dr Greg Ebert and colleagues at the institute used their studies of the behaviour of hepatitis B virus in infected cells as a basis for the treatment. The research was published today in two papers in the journal Proceedings of the National Academy of Sciences.
Dr Pellegrini said the treatment was successful in curing infections in preclinical models, leading to a human trial that began in December 2014. "We were 100 per cent successful in curing HBV infection in hundreds of tests in preclinical models," Dr Pellegrini said.
"Birinapant enabled the destruction of hepatitis B-infected liver cells while leaving normal cells unharmed. Excitingly, when birinapant was administered in combination with current antiviral drug entecavir, the infection was cleared twice as fast compared with birinapant alone. We are hopeful these promising results will be as successful in human clinical trials, which are currently underway in Melbourne, Perth and Adelaide."
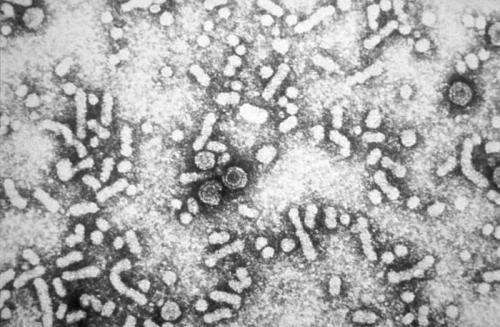
The combination treatment, developed in collaboration with TetraLogic Pharmaceuticals based in Malvern, Pennsylvania, US, targets the cell signalling pathways that the hepatitis B virus uses to keep host liver cells alive.
Chronic infectious diseases such as HBV live within the host's cells, enabling them to persist within the body for many months or years, Dr Pellegrini said.
"Normally, liver cells would respond to infection by switching on a signal that tells the cell to destroy itself 'for the greater good', preventing further infection," he said. "However our research showed that the virus commandeers the liver cells' internal communications, telling the cells to ignore the infection and stay alive. Birinapant flips the cell survival 'switch' used by the virus, causing the infected cell to die."
More than two billion people worldwide are infected with hepatitis B and approximately 400 million have a chronic HBV infection. The virus infects liver cells and can lead to complications including cirrhosis and liver cancer, resulting in more than 780,000 deaths annually.
Treatments that enable the host cell to rid itself of the virus, rather than targeting the virus itself, may prevent drug-resistant strains of HBV emerging, Dr Pellegrini said. "It is relatively easy for an organism to adapt to a drug, but it is very difficult to adapt to a change in the host cell," he said. "The virus relies on the survival mechanisms of the host, so if it can't exploit them, it dies. Such a monumental change in the virus' environment may be too big a hurdle for it to adapt to."
Dr Pellegrini and colleagues will now investigate if the same strategy could be applied to other chronic infectious diseases. "Pathogens that infect and reside inside host cells, including viral diseases such as HIV, herpes simplex and dengue fever, and bacterial infections such as tuberculosis, could all potentially be cured in a similar way," he said.
Patients are currently being recruited for the clinical trial in Melbourne by Nucleus Network, situated at the Alfred Hospital; in Perth by Linear Clinical Research, located at Sir Charles Gardiner Hospital; and in Adelaide by IDT CMAX, situated at the Royal Adelaide Hospital.
More information: Cellular inhibitor of apoptosis proteins prevent clearance of hepatitis B virus, PNAS, www.pnas.org/cgi/doi/10.1073/pnas.1502390112
Eliminating hepatitis B by antagonizing cellular inhibitors of apoptosis, PNAS, www.pnas.org/cgi/doi/10.1073/pnas.1502400112