Researchers using ground-breaking stem cell technology to test and assess new approaches to disease

Scientists have successfully used stem cells to grow fully functional bile ducts in the lab, which could one day help prevent liver tissue damage. Bile ducts are vital to enabling the liver to dispose of waste; malfunctioning bile ducts are behind a significant proportion of all liver transplants (30 % for adults and 70 % for children). The treatment will next need to be extensively tested in clinical trials before it can be used on patients.
The study, which was recently published in the scientific journal Nature Biotechnology, was made possible thanks to the TISSUEGEN project. This project, which began in 2012, sought to develop an 'in vitro' (in the lab) platform that will help scientists to develop new regenerative medicine therapies.
The platform is based on the in vitro generation of human tissue cultured from human induced pluripotent stem cells (IPSCs). These are cells that can be generated directly from adult cells, and this opens the door to a virtually limitless supply of a patient's own cell types to regenerate tissue and organs while avoiding the ethical concerns associated with using stem cells from embryos.
Liver tissues were the focus of TISSUEGEN due to their scientific and commercial significance. During the first stage of the four-year project, which is due for completion at the end of 2015, partners produced an IPSC library from an inherited metabolic liver disorder donor set, and developed key parameters of human pluripotent stem cell culture. These cells, along with human hepatocytes – cells that make up between 70 and 85 % of the liver's mass – were then loaded onto the 3D liver tissue platform.
Bioreactors were constructed using a range of innovative microfluidic techniques to produce systems compatible with analysis systems commonly used in laboratories worldwide. A key benefit of these new systems is that they allow regenerative therapies to be developed and tested on batteries of human tissues in the laboratory in a rapid, cost effective manner.
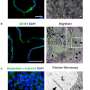
To demonstrate that the cells grown in the lab were indeed forming bile ducts, the researchers looked for characteristic markers and functions of the cells. They then compared these with samples from human donors and found that they were almost identical. This suggests that IPSC-derived hepatocytes produced from diseased donors can indeed be used to produce optimised models, in which genetic diseases can be faithfully recreated in human tissue.
The approach being pioneered by TISSUEGEN could offer scientists and medical professionals the opportunity to better understand how organs grow and develop, along with a greater understanding of disease. The platform will also enable the testing of new drugs, and means that regenerative therapies can be assessed in a scalable, cost-effective format. The 3D modelling of cancer tissue is also a possibility, leading eventually to more targeted and effective therapies.