The physician "brain drain" from sub-Saharan Africa to the US
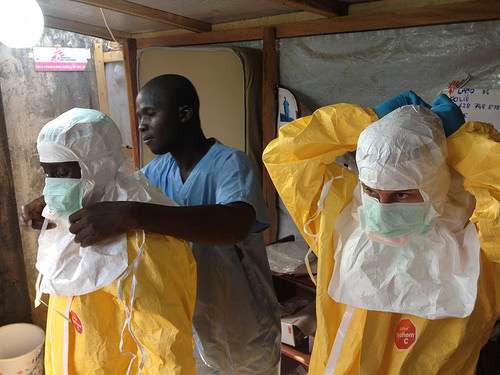
A recent PLOS One research article, "Monitoring Sub-Saharan African Physician Migration and Recruitment Post-Adoption of the WHO Code of Practice: Temporal and Geographic Patterns in the United States," examined how the migration of physicians from sub-Saharan Africa to the United States for work has led to a dire health worker shortage in the region.
While this "brain drain" has been ongoing for decades, the Ebola epidemic in West Africa demonstrated its highly damaging impact, as affected nations struggled to respond to the epidemic with weakened health systems and a limited health workforce.
From the research article… Introduction:
- The WHO database [83] indicates that there were a total of 103 physicians in Liberia in 2004, but only 51 physicians in 2008, a 50.5% total physician loss within four years. We do not have the most current counts of physicians available in Liberia because they have not been updated in the WHO database since 2008. But, we do know that the current Ebola epidemic has further depleted Liberia's meager health workforce. The Ebola Situation Report of March 18, 2015 indicates that 180 out 372 health workers infected in Liberia have died from the Ebola virus disease [86].
- We sought to monitor the post-WHO CoP [Global Code of Practice; 2010] migration of physicians originating from Sub-Saharan Africa (SSA), the region of greatest need, and recruited into the physician workforce of the US. We chose the US as the country with the largest global stock of IMGs in its workforce [44–45]. We captured all SSA immigrant physicians in residency or licensed practice in the US three years post-adoption of the CoP. We then described their growth rates, location patterns, and projected numbers in 2015.
- Those monitored included 11,787 active and semi-retired SSA-origin physicians.
From the research article… Discussion:
- Although comprising only 1.3% of the US physician workforce, SSA migrant physicians found in the December 2013 AMA Masterfile represent a significant loss for the health systems in the SSA region.
- Compared to SSA countries, populous source countries with a tradition of medical migration like India, Pakistan, and the Philippines have much larger numbers of émigré physicians in doctor-receiving countries like the US, the UK, Canada, or Australia [44]. But, relative to the number of physicians remaining in the source countries, the SSA region as a whole has a much higher migration proportion, losing between 13.9% [44] and 28% [6] of its physicians."
Why young SSA doctors leave or stay (from the research article):
- The primary motivations for young doctors to leave their home countries include: family reunifications (meeting/re-uniting with significant others in the United States); moving to the US to seek treatment for one's child; better conditions of service and standards of living; cultural trends and ease of international travel; i.e. emigrating because one can.
- As for reasons to remain in one's home country the authors identified: place attachment, professional stability and relative comfort (e.g., "It is not all rosy here in Nigeria, but one cannot go on complaining that things are terrible"); risk aversion; and, inability to obtain travel visa.
Selected Q&A with lead author "Benjamin" Tankwanchi
(Interviewed by Sara Kassabian, PLOS Social Media Coordinator)
PLOS: For a previous article, you interviewed fraternal twin brothers from Ghana who are both physicians, but chose to practice medicine in different settings. What were the factors that motivated one brother to stay in Ghana and practice medicine? What were the factors that motivated the other brother to come to the United States? Are some of their motivations to practice medicine at home or in another country generalizable to the broader group of physicians born in sub-Saharan Africa that make these choices?
AT: Yes, I interviewed two fraternal twins who are both Ghanaian-born and trained physicians with over 20 years of experience each. It must be said that these twins were raised together and accomplished almost everything together, including a mutual decision to turn down a highly selective scholarship to pursue engineering training in the UK. They instead sought admission into the medical school of their local university, the Kwame Nkrumah University of Science and Technology (KNUST) in Kumasi, Ghana.
They graduated in the early 1990's and practiced in Accra (Ghana's capital) until the late 1990's when one of twins moved to Canada to re-unite with his family (wife and first child). He now lives in an affluent suburb of the Washington DC Metropolitan Area and works as a medical faculty at one of the medical schools in the region. Interestingly, the other twin has decided to stay and practice in Ghana despite encouragements from his US-based twin brother to follow him to the US. What he explained to me was that he didn't want to become "second-class citizen" in the United States and had no desire to go through the hassles of US residency admissions. When I asked if, at times, he didn't have any regrets for his decision to stay in Ghana while his brother is practicing in much better conditions in the US and earning much more money, he observed:
"It's a dilemma for most doctors when they have to choose to leave. As I speak to you now, there are chances I've received calls [voice messages] from many of my colleagues abroad begging me to go and take care of their relatives [here in Ghana]… A lot of people are running into me and wonder why I'm still here, especially when my brother is out there [in the US]. They just can't understand."
This story challenges both societal expectations and prominent migration theories. It is not because this Ghanaian physician is unaware of the income differential between his US-based twin brother and him that he decided to practice in Ghana. It is certainly not because he lacked opportunity to emigrate or did not possess a network or migration channel to the US that he decided to stay put in Ghana. In essence, he seemed fully aware of the potential financial benefits of migration, but also of the costs. Having graduated from medical school 20 years ago, and having completed specialization training in internal medicine locally, he saw no benefits of moving to the US. He appeared quite content about his decision to stay in Ghana despite the challenging conditions of service and inadequate remuneration. "There is no place like home," he told me repeatedly.
While this was the only pair of twins I interviewed, they were not the only twins within my sample. I interviewed two additional twins, and they both reported that their twins have also migrated. Thus, I don't think that the case study of this pair of fraternal twins is generalizable. However, the main migration and non-migration factors they cited fall within one of the following categories of factors/reasons reported by participating physicians of my sample.
PLOS: Ebola was a major focus of programming at the 68th World Health Assembly in May. How much did the global health community focus on the mass exodus of physicians born in West Africa who move to the United States to practice medicine? Has the discussion about health systems weakened by Ebola led to any substantial action to improve training and retaining health workers in country?
AT: Indeed, Ebola was a dominant topic at the 68th WHA, [although I did not attend] I am unaware of any discussions focusing exclusively on the physician brain drain from West Africa to the United States.
From my reading of WHO Strategic Response Plan to the Ebola outbreak, the priority with regard to workforce has been given to the rebuilding of short-term health workforce via emergency hiring, in-service workforce training, and timely payment of health workers.
Although the United States may be the main destination for migrant skilled health workers from developing countries, it is not the only or even the main destination for many West African migrant physicians. Most countries in West Africa, including Ebola-stricken Guinea, are French-speaking. So, many of their skilled health workers practicing abroad are likely found in France and other French-speaking Western nations like Belgium.
The focus cannot be on the United States alone, although it is the big 'culprit.'
PLOS: Since the publication of your paper, has the detrimental role of the United States and other physician-receiving countries been acknowledged by global political leadership/WHO?
AT: The detrimental role of the United States and other major doctor-receiving countries has been recognized by WHO well before the publication of my papers. The strongest critique to date of the health workforce brain drain may be found in the seminal World Health Report 2006:
"When large numbers of doctors and nurses leave, the countries that financed their education lose a return on their investment and end up unwillingly providing the wealthy countries to which their health personnel have migrated with a kind of 'perverse subsidy'. Financial loss is not the most damaging outcome, however. When a country has a fragile health system, the loss of its workforce can bring the whole system close to collapse and the consequences can be measured in lives lost. In these circumstances, the calculus of international migration shifts from brain drain or gain to 'fatal flows'."
More information: "Monitoring Sub-Saharan African Physician Migration and Recruitment Post-Adoption of the WHO Code of Practice: Temporal and Geographic Patterns in the United States." PLoS ONE 10(4): e0124734. DOI: 10.1371/journal.pone.0124734
This story is republished courtesy of PLOS Blogs: blogs.plos.org.
















