Pluripotent stem cells help ID method of treatment for inherited disease
Using pluripotent stem cells, researchers at the University of Cincinnati (UC) College of Medicine and Cincinnati Children's Hospital Medical Center have gained insight into an inherited pediatric disease and identified a novel method of treatment.
Their findings are detailed July 20, 2015, online ahead of print in the Journal of Clinical Investigation, a peer-reviewed journal published by the American Society for Clinical Investigation. Jose Cancelas, MD, PhD, a professor of pediatrics at the UC College of Medicine and deputy director at Hoxworth Blood Center, is the corresponding author.
Cancelas and his colleagues focused on severe congenital neutropenia (SCN), a condition that causes affected individuals to be prone to recurrent infections. According to the National Institutes of Health (NIH), people with severe congenital neutropenia have a shortage of neutrophils, a type of white blood cell that plays a role in inflammation and fighting infection.
Patients with this disease have benefited since 1987 from the long-term administration of granulocyte colony-stimulating factor (G-CSF) which has significantly reduced the mortality associated with infections. However, as most patients with SCN are now escaping death from sepsis due to G-CSF therapy, physicians are realizing a risk of one in four patients to develop leukemia at 15 years of G-CSF therapy. Therefore, there is a need to find alternative therapies for these patients.
"A lack of appropriate models to recapitulate SCN has substantially hampered the understanding of the genetic etiology and pathobiology of this disease, which is required to develop targeted therapies acting on pathogenetic mechanisms of disease," Cancelas says. "We were able to generate both normal and SCN patient-derived induced pluripotent stem cells to perform our research."
Induced pluripotent stem cells, or iPSCs, are called pluripotent because of their ability to become any of the more than 200 different cell types in the human body. iPSCs can be generated from the cells of individual patients, and therapeutic cells derived from those iPSCs would have that person's genetic makeup and not be at risk of rejection.
According to the NIH, SCN can result from mutations in at least five different genes. These genes play a role in the maturation and function of neutrophils, which are cells produced by the bone marrow that secrete immune molecules and ingest and break down foreign invaders. About 60 percent of all cases of SCN, Cancelas says, are caused by mutations in the ELANE ("elastase, neutrophil expressed") gene, which encodes neutrophil elastase.
"With iPSC lines, we have a renewable source of patient-derived cells to study the cellular mechanisms of disease and explore novel therapies with the purpose of personalized medicine," Cancelas says. "This is of immense value in studying genetic diseases that cannot be recapitulated in animal models."
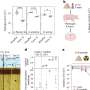
By studying the patient-derived iPSC lines and comparing them with normal iPSC lines, Cancelas and his colleagues found that pathogenesis of ELANE point mutations was associated with neutrophil elastase mislocalization, which in turn triggered dysfunctional survival signaling. The drug sivelestat, an inhibitor of neutrophil elastase, restored normal intracellular neutrophil elastase localization.
"With the knowledge that the disease pathogenesis of severe congenital neutropenia pivots upon neutrophil elastase mislocalization, we propose that our work provides a paradigm that can be clinically exploited to achieve therapeutic responses by using sivelestat in combination with small-molecule targeting to correct neutrophil elastase mislocalization," Cancelas says.
More information: "Pathogenesis of ELANE-mutant severe neutropenia revealed by induced pluripotent stem cells." www.jci.org/articles/view/80924