A conversation with Nobel prize-winning neuroscientist Dr. Eric R. Kandel
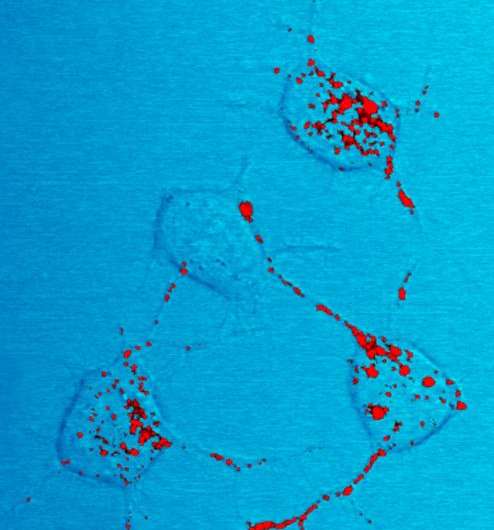
Posttraumatic Stress Disorder (PTSD) has been described as a disorder of memory. It has become quite apparent that there are two types of memory in PTSD: the first being the involuntary intrusions of the trauma, and the second being the voluntarily recalled memories that constitute the trauma story, also known as the trauma narrative. Both are fundamentally different in their quality and form.
The involuntary intrusions are vivid, highly emotional, and involve a sense of reliving the original trauma. In contrast, the voluntarily recalled trauma narratives do not share this same intensity, but their content is notable for being significantly disorganized. Such disorganization can be found very soon after the traumatic event and hence is not attributable to poor recall, but to the very nature of these traumatic memories themselves.
In essence, there is an inability to put into words the most emotional part of a traumatic event, a period of time which could have lasted anywhere from several seconds to several hours. Traumatic memories are also unstable, so what is under voluntary and involuntary control varies over time. For this reason, the recall of trauma over different points in time creates different trauma accounts, with such discrepancies being more noticeable as the symptoms of PTSD become more severe.
For such disorders of memory, a natural follow up question is what are the molecules and chemical building blocks that our memories are made from? Unlike taking a blood sample, a saliva swab or a sample of bone marrow, there is no simple way to sample brain tissue from a live human. For this reason, neuroscientists have relied on animal models to discover what goes on in the brain when memories are made.
The work of Eric R. Kandel forms the basis for much of what we understand about how memories are formed. Dr. Kandel was awarded the 2000 Nobel Prize in Physiology or Medicine for his extensive body of pioneering work investigating the synaptic connections between nerve cells in sea slugs. His work has illuminated some of the basic molecular mechanisms underlying learning and memory in animals and is central to understanding not only normal memory, but also disorders that affect memory, such as PTSD.
More recently, Dr. Kandel and his colleagues identified a molecule, a prion protein called CPEB, (cytoplasmic polyadenylation element-binding protein 3) that plays a key role in the maintenance of long-term memories in the sea slug Aplysia and in mice. In a 2015 study, Kandel and his colleagues trained mice to memorize a way to navigate through a maze, then the researchers knocked out the mouse homolog of the CPEB gene called CPEB3 and this knocked out the maintenance of long-term memories and caused the mice to forget how to navigate the maze.
Dr. Kandel is a Professor at Columbia University, the Kavli Professor and Director of the Kavli Institute for Brain Science, Co-Director of the Mortimer B. Zuckerman Mind Brain Behavior Institute and a Senior Investigator at the Howard Hughes Medical Institute. I spoke with him about this recent publication and the relevance of such findings to disorders of memory, such as PTSD.
Dr. Jain: The first question I had was about prions. They have a really bad reputation in the world of medicine as being associated with horrific diseases like Creutzfeldt-Jakob Disease (CJD) and Bovine Spongiform Encephalopathy (BSE). Your work has shown that in order to maintain long term memory, we need local protein synthesis at the synapse. You and your colleagues have identified the CPEB protein as a functional prion which has this role of keeping memory indefinitely. Could you talk a little bit more about functional prions and how they differ from prions that cause pathological changes in the brain?
Dr. Kandel: Well, functional prions differ from pathological prions in two ways. First, in pathological prions, the conversion from the soluble form to the aggregated self-perpetuating form is spontaneous. In functional prions, it is regulated by a physiological signal. Secondly, in pathological prions, once the prions assume an aggregated self-perpetuating form, prion proteins then kill the cell. They are then released by the dying cell and taken up by other cells, they kill the next cell and are passed on from one cell to another like an infection. The functional prions are not only turned on by a physiological signal, but when they are turned on and reach the aggregated self-perpetuating form that is their normal function. They are inactive when they are not in the aggregated form. So they fulfill their normal function, which in this case is regulating local proteins synthesis.
Dr. Jain: Taking this one step further, when we think specifically about a psychiatric disorder, such as PTSD, can you speak a little bit as to what these recent findings mean in terms of understanding what the molecular basis for PTSD might be?
Dr. Kandel: Before we come to PTSD, think of anything that involves memory loss or age related memory loss that, in fact, has steps that are upstream from CPEB. This is important also for age related memory loss. The same functional prion that I spoke about.
PTSD very likely has prion mechanisms. Joseph Rayman in our lab identified a second prion in addition to CPEB that seems to play a role as a protective factor in PTSD. We have not done enough to talk about it and it has not been published yet.
Dr. Jain: Neuroscience data comes from studies using animal models (sea slugs, mice etc.). Can you speak a little bit to those of us who are not so familiar with cutting edge neuroscience methodologies, how do we infer from animal models what might be happening in the human brain?
Dr. Kandel: Well, one cannot be certain unless one explores the molecules directly in the human brain, but there is a homologue in the human brain. There is no obvious reason for thinking it does not have a similar function, but until one tests it one cannot know for sure.
Dr. Jain: We hear about these amazing discoveries about these prions and homologues in humans. What is your vision for how basic science research will actually translate clinically into impacting people living with memory disorders?
Dr. Kandel: We are already there in some areas. We have far to go in other areas, but I will give you an example. We have a pretty good understanding of Alzheimer's disease. We know the toxicity of beta amyloid. We do not know why the drugs that are directed against beta amyloid do not work, but one possibility that is being seriously entertained is that by the time the patient comes to see a physician, they have had the disease for ten years. That is a very long time and you lose a lot of nerve cells in ten years, and drugs do not bring nerve cells back once they are dead.
We need to diagnose the disease earlier and a major effort now, in Alzheimer's research, is early diagnosis. Imaging, cerebral spinal fluid, genetic warning signals etc.
The other thing is it has proven possible to define an independent disorder, age related memory loss. Recent work from our lab, and that of Scott Small, ,has shown there is a separate entity, independent of AD, called Age Related Memory Loss. We have identified the molecular pathways involved in that disorder. We have treatments that work very effectively in animals. I think the time is going to come soon when these will be tried in people.
All of these came out from a basic science and work with experimental animals. So even though we are in the very early stage of understanding the really complex functions of the brain, we are making progress and all of this will hopefully have some therapeutic impact.
This story is republished courtesy of PLOS Blogs: blogs.plos.org.