Seizures in neonates undergoing cardiac surgery underappreciated and dangerous
With mounting concerns about postoperative seizures, doctors at The Children's Hospital of Philadelphia placed 161 neonates who had undergone cardiac surgery on continuous EEG monitoring. They found that 8% of the neonates experienced EEG seizures and 85% of these were unrecognized clinically. Many of the seizures were severe, and the seizure group faced a higher risk of death, according to a report in The Journal of Thoracic and Cardiovascular Surgery, the official publication of the American Association for Thoracic Surgery (AATS).
"In their article, Naim and colleagues have clearly pointed out that if we don't carefully assess for seizure activity with EEG monitoring, we will not identify these at-risk neonates," stated Carl L. Backer, MD, Division of Cardiovascular-Thoracic Surgery, and Bradley S. Marino, MD, MPP, MSCE, Division of Cardiology, both at the Ann & Robert H. Lurie Children's Hospital of Chicago, in an accompanying editorial. "It is clearly no longer adequate for investigators reporting outcomes after neonatal cardiac surgery to state that neonates did not have postoperative neurologic complications if they do not use continuous EEG monitoring."
Conducting a quality improvement project, the team at The Children's Hospital of Philadelphia implemented continuous EEG monitoring in neonates (? 30 days corrected gestational age) following cardiac surgery for repair of congenital heart disease. During an 18-month period from June 15, 2012 to December 31, 2013, records of continuous EEG (CEEG) were obtained from 94% (161) of 172 surgeries.
CEEG began within six hours of the patient returning to the cardiac intensive care unit after surgery. Monitoring continued for 48 hours if no seizures were detected and for 24 hours after the last seizure if a seizure occurred. EEG technologists were present for EEG monitoring and interpretation at all times.
The neonates had a range of cardiac defects, with 42% class I (two ventricles with no aortic arch obstruction), 22% class II (two ventricles with aortic arch obstruction), 9% class III (single ventricle with no aortic arch obstruction), and 27% class IV (single ventricle with aortic arch obstruction). A variety of repairs were performed, including stage I Norwood (27%) and arterial switch operations (16%).
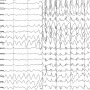
Bedside clinicians identified events such as abnormal body movements, hypertension, or tachycardia in 32 neonates - but none of these events had associated abnormal EEG activity. However, 13 of the 161 neonates (8%) had EEG seizures. Of these, 85% (11) were not detected clinically. "This indicates that bedside clinical assessment for seizures without CEEG is unreliable," explained lead investigator Maryam Y. Naim, MD, Division of Cardiac Critical Care, Departments of Anesthesiology and Critical Care Medicine and Pediatrics, The Children's Hospital of Philadelphia, and Assistant Professor, Perelman School of Medicine at the University of Pennsylvania.
When seizures occurred, they were severe. Sixty-two percent of the neonates with seizures experienced status epilepticus, a dangerous condition in which either a single seizure lasts more than 30 minutes or recurrent seizures together last for more than 30 minutes within a one-hour block.
Dr. Naim and colleagues found that the occurrence of seizures in this patient group was "ominous because 38% (5/13) of neonates with postoperative seizures died" (compared to 3% of those who did not have seizures). Indeed, seizures appear to be a marker of brain injury, since many of those with seizures had diffuse or multifocal lesions apparent on MRI or ultrasound. In the editorial, Dr. Backer and Dr. Marino commented, "Although this may have been a result of increased severity of disease and comorbidities, the prevention of postoperative seizures is still an important goal, which can only be achieved if we monitor for seizures and then use assessment of various surgical and postoperative management strategies to eliminate the development of seizures."
The investigators looked for predictors of seizure occurrence. They found that surgical factors such as delayed sternal closure and longer deep hypothermic circulatory arrest duration were associated with an increased seizure risk. Seizures were also more frequent in neonates who subsequently required extracorporeal membrane oxygenation or experienced cardiac arrest.
Dr. Naim believes that postoperative CEEG is warranted to identify seizures because they are associated with worse neurodevelopmental outcomes. Recognizing seizures opens treatment with medications or other therapies to reduce seizure occurrence. Dr. Naim acknowledged that there is a lack of high-level data demonstrating that seizure treatment can improve outcomes in high-risk children, such as those undergoing cardiac surgery. However she cited the findings of the Boston Circulatory Arrest Study that showed that postoperative seizure occurrence was the medical variable most consistently related to worse long term neuropsychologic outcomes.
Dr. Backer and Dr. Marino raise another pragmatic issue: the costs and manpower required for CEEG, such as EEG technologists 24/7 and use of comprehensive 12-scalp electrode monitoring. "This level of sophisticated monitoring, of course, is not available at all institutions. What we need is a screening tool that is not as labor intensive. This would remove the expense and staffing associated with full EEG monitoring for the 92% of patients who do not have seizures."
More information: "Subclinical seizures identified by postoperative electroencephalographic monitoring are common after neonatal cardiac surgery," by Maryam Y. Naim, MD, J. William Gaynor, MD, Jodi Chen, MD, Susan C. Nicolson, MD, Stephanie Fuller, MD, Thomas L. Spray, MD, Dennis J. Dlugos, MD, Robert R. Clancy, MD, Livia Vianez Costa, MD, Daniel J. Licht, MD, Rui Xiao, PhD, Heather Meldrum, RN, and Nicholas S. Abend, MD. DOI: dx.doi.org/10.1016/j.jtcvs.2015.03.045