Discovery could lead to new heart disease treatments
By tracking a single cell in a growing heart, scientists from Stanford University have discovered a cell type that could repair damaged arteries.
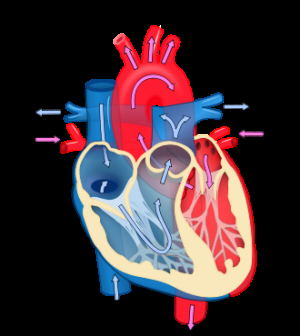
Coronary artery disease is the leading cause of death worldwide, but there is currently no effective method to regenerate new coronary arteries in diseased or injured hearts. The findings in the journal eLife identified a progenitor cell type that could make it possible.
The study was carried out with mice but, as the blood vessels of the human heart are similar, it could lead to new treatments for the disease or to restore blood flow after a heart attack.
"Current methods to grow new blood vessels in the heart stimulate fine blood vessels rather than re-establishing the strong supply of blood provided by the main arteries. We need arteries to restore normal function," says senior author Kristy Red-Horse from the Department of Biological Sciences.
Current efforts in treatment also often focus on the diseased heart, while the Stanford University scientists argue that it is important to first understand how the vessels of the healthy heart are built up.
"If we want to regenerate diseased hearts, we need to first understand how the heart creates the building blocks of healthy coronary arteries," says lead author Dr. Katharina Volz, the first PhD graduate in Stem Cell Biology and Regenerative Medicine at Stanford University.
"Our study describes step-by-step how coronary arteries develop in the embryonic mouse heart."
It was already known that smooth muscle is formed from cells in the epicardium, the layer that covers the heart. During embryonic development, many epicardial cells travel deeper into the wall of the heart and some form smooth muscle. But the original cell type that undergoes this transition, and the signals that trigger differentiation into smooth muscle, were poorly understood.
The team can now reveal that the smooth muscle of the arteries is derived from cells called pericytes. The small capillary blood vessels throughout the developing heart are covered in pericytes. They receive signals through a protein called Notch 3 to differentiate and form the smooth muscle covering needed for larger artery walls.
Pericytes are also found throughout the adult heart which suggests that they could be used to trigger a self-repair mechanism. When the main arteries become blocked and a person suffers a heart attack, small collateral vessels can form a detour around the blockage. Large collateral arteries are required to provide significant blood flow to healing tissues. Providing the right molecular signals to turn pericytes into smooth muscle cells may promote a transition from tiny blood vessels to true arteries in the healing heart.
A problem with cell or tissue transplantation can be that the cells don't integrate or they differentiate into slightly different cells types than intended. As pericytes are spread all over the heart on all the small blood vessels, they could be used as a target to stimulate artery formation without the need for transplantation.
The team is now investigating whether pericytes differentiate into smooth muscle as part of this process and whether it can be activated or sped up by introducing Notch 3 signalling molecules.
"Now that we are beginning to really understand coronary artery development, we have initiated studies to reactivate it in injury models and hope to some day use these same methods to help treat coronary artery disease," says Red-Horse.