Researchers test 'smart' simulations to analyze unknown variables in immune response
Technology to predict how our bodies will manage chronic diseases such as Crohn's disease and inflammatory bowel disease promises to accelerate the discovery of new treatments, identify leads for further study, and occasionally uncover hidden knowledge about how our immune system operates.
Researchers at the Virginia Bioinformatics Institute at Virginia Tech's Center for Modeling Immunity to Enteric Pathogens recently released a study in the open-access journal BioData Mining evaluating a set of these streamlined approaches for modeling our immune system—techniques employing a facet of artificial intelligence known as machine learning.
Building on the analytical power of linear equation models, these systems get "smarter" as they're provided with more information, picking out patterns in the data that can be used to make sense of unknown variables in the immune response.
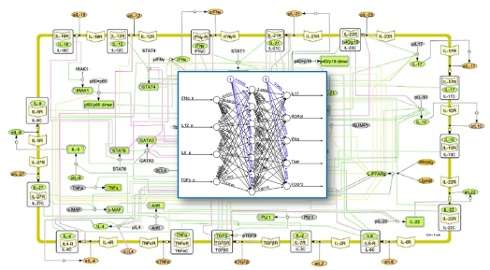
The complexity of the immune system presents a serious challenge to researchers who want to mathematically model its behavior. Cells that help regulate the immune system such as CD4+ T cells can differentiate into at least nine cell subsets, each of which plays its own unique role in orchestrating the body's response to infection.
Traditional models would require each of those cellular behaviors to be painstakingly represented as elements of a linear equation for a simulation to return accurate results—a time-consuming process which leaves the system ill-equipped to factor new or unexpected variables into its calculations.
"For a long time, computational models were only as intelligent as we could program them to be, limiting their application to a defined set of biological functions," said Vida Abedi, assistant professor at the Nutritional Immunology and Molecular Medicine Laboratory. "The 'intuitive' logic of machine learning means their scope isn't set in advance—the same model could theoretically be scaled up from the cellular level all the way to the individual, human populations, and their environment."
This test of machine-learning methods was spearheaded by researchers in the Center for Modeling Immunity to Enteric Pathogens, a $12 million National Institute of Allergy and Infectious Diseases-funded resource dedicated to developing, validating, and disseminating user-friendly models for studying the immune responses in the gut.
The team compared multiple approaches and found that one particular advanced machine learning method, Artificial Neural Networks, could quickly be "trained" to predict the differentiation of CD4+ T cells.
Building on recent successes in developing tools capable of modeling complex interactions in the gut's mucosal immune system, the team hopes that further applications of machine learning could personalize their predictive power to meet the needs of specific individuals.
"No two people experience the same Crohn's disease—genetics, environment, microbiome, nutrition, and medical history all play a role in how it is felt and how it should be safely managed," said Josep Bassaganya-Riera, director of the Nutritional Immunology and Molecular Medicine Laboratory. "Advanced machine learning methods make it easier to consider all of those specific circumstances together, getting us a step closer to models that provide comprehensive and accurate predictions of each individual's response to illness and can inform the development of precision medicine interventions and predict the success of human clinical trials."