Inflammation markers could guide depression treatments

Psychiatrists investigating depression have been energized in recent years by reports of rapid, successful treatment with drugs that interfere with the brain chemical glutamate, such as the anesthetic ketamine.
New research from Emory University School of Medicine is providing hints as to which forms of depression may respond best to drugs that target glutamate.
The findings are scheduled for publication online on January 12 in Molecular Psychiatry.
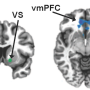
Depressed patients with signs of systemic inflammation have elevated levels of glutamate in regions of the brain that are important for motivation, the researchers have found.
"Our results suggest that inflammation markers can guide us to which depressed patients respond best to glutamate blockers," says lead author Ebrahim Haroon, MD, assistant professor of psychiatry and behavioral sciences at Emory University School of Medicine and Winship Cancer Institute. "This could be an important step toward personalizing treatment for depression."
Glutamate is a chemical messenger used by neurons to communicate. However, at high levels, it can become toxic to both neurons and glia, cells that support brain health. It is unlikely that the elevated levels seen in some depressed patients are acutely toxic, Haroon says.
"Still, we think that one of the ways that inflammation may harm the brain and cause depression is by increasing levels of glutamate in sensitive regions of the brain, possibly through effects on glia," he says.
Researchers examined 50 patients with depression who were not receiving antidepressant medication at that time. Inflammation was determined by a blood test for C-reactive protein (CRP), which was measured on repeat visits to make sure its levels were stable.
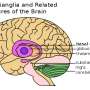
The team used an imaging technique called magnetic resonance spectroscopy (MRS) to measure glutamate levels in the basal ganglia, a brain region important for motor control, motivation and decision making. The researchers also measured levels of myo-inositol, a marker of glial health.
High glutamate and myo-inositol levels in the basal ganglia were associated with patients' reports of anhedonia, an inability to experience pleasure, and slow motor function, as measured by finger tapping speed.
"We focused on the basal ganglia because we had previously seen that a treatment for hepatitis C virus that arouses inflammation and can trigger depressive symptoms could also increase glutamate levels there," Haroon says.
He adds that the paper's findings do not directly address how ketamine and other glutamate-targeting drugs may work against depression, but may indicate which patients would be likely candidates.
A previous study of people with difficult-to-treat depression found that only those with high inflammation markers tended to improve in response to the anti-inflammatory antibody infliximab.
More information: E Haroon et al. Conceptual convergence: increased inflammation is associated with increased basal ganglia glutamate in patients with major depression, Molecular Psychiatry (2016). DOI: 10.1038/mp.2015.206