Stroke patients' speech loss linked to loss of brain interconnections
When brain regions that control speech and reading comprehension are destroyed due to blockage of blood flow, patients are often unable to speak or comprehend spoken or written language. These difficulties with language, or "aphasia," are a common symptom in the aftermath of stroke. However, in a new study published in Restorative Neurology and Neuroscience, researchers report that damage to the underlying connections among different areas of the brain can also affect the severity of aphasia.
The brain's macro architecture of connections can be reproduced as a "connectome" composed of nodes representing various regions of the brain and their edges, the connections between such nodes. Some of these nodes function as hubs, which are fundamental to the overall organization and distribution of information throughout the brain. When a network hub has an excess of interconnections, it is part of a so-called "rich club network." There is a growing body of evidence that damage to this rich club network can impair various speech and reading functions in much the same way as direct damage to brain regions normally associated with speech and comprehension.
This investigation involved 44 patients who had experienced a left hemisphere ischemic stroke at least six months prior to the study. Aphasia testing used the Western Aphasia Battery, which determined overall aphasia severity, as well as sub-assessments of speech fluency, auditory comprehension, speech repetition, and naming. Each participant was assigned an Aphasia Quotient (WAB-AQ) as a measure of severity. MRI Diffusion Tensor Imaging (MRI-DTI), which can map the interconnections between brain regions, was used to identify the rich club network in each individual patient.
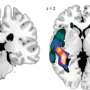
Investigators found that when imaging revealed that the post-stroke patients studied had different distributions of rich club nodes, their aphasia could differ markedly. They present a striking example in which two patients had similar volumes of stroke damage but very dissimilar numbers of rich club nodes remaining nearby. Patient B had more severe aphasia (lower WAB-AQ = 23.6) than patient A (WAB-AB = 64.6).
"Subjects whose spared cortical language regions are integrated into the remaining network as rich club nodes are less likely to have more severe forms of aphasia," explained lead investigators Ezequiel Gleichgerrcht, MD, PhD, and Leonardo Bonilha, MD, PhD, from the Department of Neurology, Medical University of South Carolina.
While clinical practice has often focused on the direct damage to the grey matter of the brain, new mapping techniques such as MRI-DTI can examine the white matter connections throughout the brain. The investigators stressed that, "These findings further highlight the potential relevance and utility of mapping the neural connectome of individual subjects. Identifying patterns of white matter integrity has the potential to add valuable information to the well-established volume-based analysis of clinical, neuropsychological, and language outcomes from both theoretical and clinical perspectives."
More information: Ezequiel Gleichgerrcht et al. Preservation of structural brain network hubs is associated with less severe post-stroke aphasia, Restorative Neurology and Neuroscience (2015). DOI: 10.3233/RNN-150511