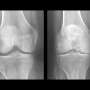
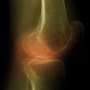
Findings do not support use of vitamin D to reduce pain from knee osteoarthritis
Vitamin D supplementation for individuals with knee osteoarthritis and low 25-hydroxyvitamin D levels did not reduce knee pain or slow cartilage loss, according to a study appearing in the March 8 issue of JAMA.
Symptomatic knee osteoarthritis occurs among 10 percent of men and 13 percent of women age 60 years or older. Currently there are no disease-modifying therapies for osteoarthritis. Vitamin D can reduce bone turnover and cartilage degradation, thus potentially preventing the development and progression of knee osteoarthritis. Observational studies suggest that vitamin D supplementation is associated with benefits for knee osteoarthritis, but current evidence from clinical trials is contradictory.
Changhai Ding, M.D., Ph.D., of the University of Tasmania, Hobart, Tasmania, Australia, and colleagues randomly assigned 413 patients with symptomatic knee osteoarthritis and low 25-hydroxyvitamin D to receive monthly treatment with oral vitamin D3 (50,000 IU; n = 209) or an identical placebo (n = 204) for 2 years. The study was conducted in Tasmania and Melbourne, Australia.
Of 413 enrolled participants (average age, 63 years; 50 percent women), 340 (82 percent) completed the study. The researchers found that vitamin D supplementation, compared with placebo, did not result in significant differences in change in MRI-measured tibial cartilage volume or a measure of knee pain over 2 years. There were also no significant differences in change of tibiofemoral cartilage defects or change in tibiofemoral bone marrow lesions. Vitamin D levels did increase more in the vitamin D group than in the placebo group over 2 years.
"These data suggest a lack of evidence to support vitamin D supplementation for slowing disease progression or structural change in knee osteoarthritis," the authors write.
More information: JAMA, DOI: 10.1001/jama.2016.1961