Non-inflammatory destructive periodontal disease
Although, bacteria are a critical etiologic factor that are needed to develop periodontal disease, bacteria alone are insuficiente to induce a periodontal disease. A susceptible host is also required, and the host's susceptibility as local and/or general predisposing risk factors, are important determinants of the disease status. An accurate diagnosis is often essential in developing a predictable and suitable treatment plan, which, when executed, gives a guide to the resolution of the periodontal disease's activity. The majority of all forms of periodontal diseases, are considered as microorganism-induced diseases, which promote an inflammatory host defense response against the bacteria and noxious materials from bacterial plaque.
The inflammatory process inactivates bacteria, but produces the liberation of bacterial and neutrophil derived products such as enzymes, which induce periodontal tissue destruction by lytic activities. Therefore, the characteristics of the most common periodontal disease are: presence of gingival inflammation, ulceration of the junctional epithelium, loss of connective tissue and alveolar bone, causing apical migration of the junctional epithelium and development of periodontal pockets.
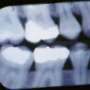
However, not all types of periodontal disease seem to be caused by periodontopathogenic bacteria, and not all are distinguished by an evident inflammatory process, and periodontal tissue destruction associated with periodontal periodontal pocket formation and progressive deepening. Non inflammatory destructive periodontal disease (NIDPD), is a severe destructive periodontal disease, which is characterized by periodontal attachment loss, alveolar bone loss, generalized gingival recession without pathognomonic sign of inflammation, and periodontal pocket development. Conventional periodontal therapy and antimicrobial therapy are ineffective, in preventing further progression of the disease.
A NIDPD case was studied in order to analyse features of the disease, and discuss the possible etiologic factors as an association of endogenous opportunist bacteria with anatomical aspects, occlusion pattern, emotional stress and mouth breathing condition.
More information: Kina José Ricardo et al, Non-Inflammatory Destructive Periodontal Disease, The Open Dentistry Journal (2016). DOI: 10.2174/1874210601610010050