Is laparoscopic repair of ventral hernia the ideal approach for all patients?
Laparascopic repair of ventral hernias has advanced and overcome many challenges during the past two decades, and patients who are obese, diabetic, and have a hernia no larger than 10 cm in width are best suited for this evolving minimally invasive approach. New types of mesh to close the defect are in development, and better long-term studies are needed to define best practices and determine ideal indications of this technique, according to an article in Journal of Laparoendoscopic & Advanced Surgical Techniques (JLAST), a peer-reviewed journal published by Mary Ann Liebert, Inc., publishers. The article is available free to download on the JLAST website until June 16, 2016.
William Tobler, Jr., MD, University of Pittsburgh, PA and Kamal Itani, MD, Boston University and Harvard Medical School, Boston MA, discuss the patient- and hernia-related factors and technical considerations that contribute to the success or failure of these procedures in the article "Current Status and Challenges of Laparoscopy in Ventral Hernia Repair."
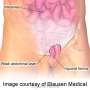
Relevant patient factors may include obesity, smoking, diabetes, cirrhosis, and cardiopulmonary disease. Hernia factors involve the size, location, and characteristics of the defect and whether it is recurrent. The authors also describe the types of mesh used, location of the mesh, and techniques for mesh fixation, as well as common complications and the use of robotic surgical approaches and other future technology.
"Laparoscopic ventral hernia repair is not free of complication and recurrence is a real possibility," says Editor-in-Chief P. Marco Fisichella, MD, MBA, Harvard Medical School, Brigham and Women's Hospital, Boston VA Healthcare System, Boston, MA. "Tobler and Itani explore the risk factors associated with this operation and highlight the concrete evidence-based indications and contraindications of the laparoscopic approach."
More information: William D. Tobler et al, Current Status and Challenges of Laparoscopy in Ventral Hernia Repair, Journal of Laparoendoscopic & Advanced Surgical Techniques (2016). DOI: 10.1089/lap.2016.0095