Photoacoustic and magnetic resonance imaging visualizes blood flow and oxygenation status in brain tumor tissue
Cancer diagnostics and therapy monitoring have moved into a new dimension through A*STAR research, which has developed a high-resolution and noninvasive approach to visualize brain tumors by combining photoacoustic with magnetic resonance imaging (MRI) techniques.
To be effective, anticancer therapies need early diagnosis and detection of malignant tumors, as well as a deep understanding of their metabolism. Current diagnosis uses in vivo imaging methods, coupling MRI and positron emission tomography (PET) at preclinical and clinical stages.
Within these methods, MRI produces detailed anatomical images of brain tumors while PET gives functional and metabolic information by detecting gamma-rays from a radioactive compound. However, PET presents a relatively low spatial resolution, and it cannot be used too long or frequently because of its radiative nature.
Now, Malini Olivo and co-workers from the Singapore Bioimaging Consortium have combined MRI with multispectral optoacoustic tomography (MSOT) instead of PET. In this non-radiative technique, laser light excites light-absorbing specimen components, causing tissues to expand thermoelastically. This generates acoustic waves, which propagate through the tissue and its surroundings before being detected and converted into ultrasound images by transducers.
"MSOT produces anatomical, functional and molecular data, while MRI offers good contrast for soft-tissue anatomy and various imaging sequences for different physiological properties," explains Olivo.
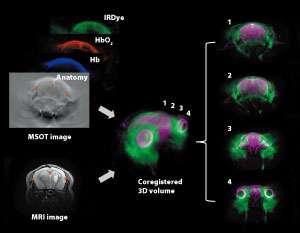
Because tumors exhibit abnormal glucose metabolism, the researchers monitored the uptake and behavior of a dye-labeled sugar analog acting as a probe in mice affected with brain cancer. They tracked the intravenously injected dye in the brain by separately acquiring MRI and MSOT images. Next, they superimposed both types of images using reference landmarks inside the brain to create a spatially correlated, or co-registered, three-dimensional volume (see image).
The dye accumulated in tumor and contralateral regions of the brain in the first hour after injection. Subsequently, it started to clear from the contralateral side but remained on the tumor side up to 48 hours post-injection. This provides a high tumor-to-normal contrast suitable for diagnostic imaging.
"This dye biodistribution can be coupled with other MRI and MSOT-derived information, such as oxygenation status and vasculature, to gain further insight into tumor physiology," says Olivo.
Olivo's team is further exploring potential applications of the multimodal approach to cancer diagnostics and therapy. "In a follow-up study, we can monitor blood vessel formation and oxygenation in tumors during their growth as well as changes in blood flow within tumors in response to anticancer drug treatments to evaluate drug efficacy," she adds.
More information: Amalina Binte Ebrahim Attia et al. Multispectral optoacoustic and MRI coregistration for molecular imaging of orthotopic model of human glioblastoma, Journal of Biophotonics (2016). DOI: 10.1002/jbio.201500321