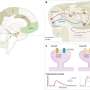
SAVE - sleep apnea treatment: No cardiovascular benefit
More than 3 years of nightly treatment with a continuous positive airway pressure (CPAP) machine did not reduce cardiovascular risk more than usual care among patients with cardiovascular disease and obstructive sleep apnea (OSA).
Findings from the Sleep Apnea Cardiovascular Endpoints (SAVE) study were presented at ESC Congress 2016, with simultaneous publication in the New England Journal of Medicine.
"Given the level of risk of cardiovascular disease attributed to OSA in previous observational studies, we were surprised not to find a benefit from CPAP treatment," said the study's principal investigator Doug McEvoy, MD, from the Adelaide Institute for Sleep Health at Flinders University in Adelaide, Australia.
The SAVE study recruited sleep apnea patients with moderate-to-severe disease from 89 clinical centres in 7 countries.
Participants were predominantly elderly (approximately 61 years), overweight, habitually snoring males - all with coronary artery or cerebrovascular disease.
A total of 2,717 individuals were randomized to receive usual care alone, or usual care plus CPAP.
To be eligible, participants had to achieve a minimum 3 hours of sham-CPAP adherence per night in a one week run-in before the study started.
Usual care included concomitant CV risk management, based on national guidelines, as well as advice on healthy sleep habits and lifestyle changes to minimize OSA.
The study showed that 42% of patients assigned to CPAP had good adherence (an average of 4 or more hours per night). Mean apnea-hypopnea index (AHI, a measure of OSA severity) decreased from 29.0 to 3.7 events per hour when patients used CPAP, indicating good control of their OSA.
However, after a mean follow-up time of 3.7 years for 1,341 usual care and 1,346 CPAP patients included in the final analysis, there was no difference between groups in the primary outcome - a composite of death from any CV cause, myocardial infarction or stroke, and hospitalisation for heart failure, acute coronary syndrome, or transient ischemic attack.
Specifically, 17.0% of patients in the CPAP group and 15.4% in usual-care had a serious CV event (hazard ratio 1.10; 95% CI 0.91 to 1.32; P=0.34).
"It's not clear why CPAP treatment did not improve CV outcomes," said Prof McEvoy.
"It is possible that, even though the average CPAP adherence of approximately 3.3 hours per night was as expected, and more than we estimated in our power calculations, it was still insufficient to show the hypothesized level of effect on CV outcomes."
Importantly though, CPAP did improve the wellbeing of participants, defined by symptoms of daytime sleepiness, health-related quality of life, mood - particularly depressive symptoms - and attendance at work.
Prof McEvoy said that "While it is disappointing not to find a reduction in CV events with CPAP treatment, our results show that treatment of OSA in patients with CV disease is nevertheless worthwhile - they are much less sleepy and depressed, and their productivity and quality of life is enhanced."
"More research is needed now on how to reduce the significant risk of CV events in people who suffer from sleep apnea," he added.
"Given our finding of a possible reduction in cerebrovascular events in patients who were able to use CPAP for more than 4 hours per night, and of prior studies showing a stronger association between OSA and stroke than between OSA and coronary artery disease, future trials should consider targeting patients with OSA and stroke who can achieve a high level of compliance with CPAP."