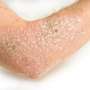
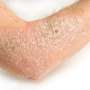
Clearing up common myths about psoriasis
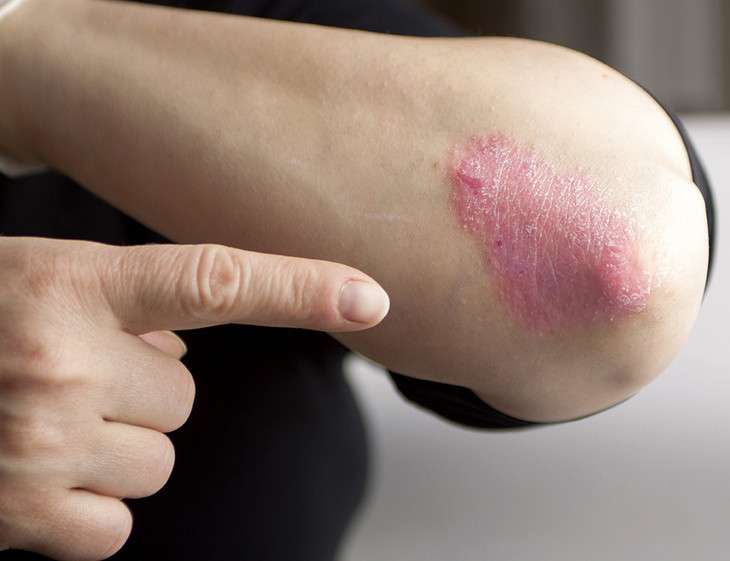
Psoriasis is a misunderstood disease, often kept under wraps by sufferers who want to hide their skin lesions. This week, Dr. Sara Ferguson, a dermatologist at Penn State Medical Group in State College, separates fact from myth about psoriasis and the various treatment options.
Myth: Psoriasis is rare.
Fact: Psoriasis affects 2 to 5 percent of the population, which means as many as 16 million Americans live with this condition. Many of them have not sought treatment from a physician because their symptoms are mild.
Myth: Psoriasis is a skin disease.
Fact: Psoriasis is a multi-system inflammatory disease of the immune system that can affect the joints. Yes, people who have psoriasis may have skin lesions or rashes that can be as small as a coin or that can involve most of their skin. Patients with psoriasis also are at higher risk for developing conditions such as heart disease, high blood pressure, diabetes, depression, psoriatic arthritis, inflammatory bowel disease and obesity. In addition to getting treatment for their skin, it's important for these patients to consult regularly with their primary care physician about other risk factors.
Myth: Psoriasis is contagious.
Fact: Psoriasis is not an infection, and it does not involve a virus or bacteria. You cannot contract it by touching someone who has it, and you can't "give" it to someone else. Psoriasis does tend to run in families, but not because they "catch" it from each other. Certain inherited genes can lead to psoriasis when a person who carries them is exposed to external triggers such as infection or skin injury.
Myth: No one can help.
Fact: Many patients who sought treatment years ago became frustrated with the limited treatment options available then. They may not realize that new treatments are available.
Myth: Topical creams are the only treatment for psoriasis.
Fact: In addition to creams, dermatologists can consider many treatment options. They include:
- Topical treatments applied to the skin, for mild to moderate psoriasis. These include corticosteroids, vitamin D, anthralin, coal tar and salicylic acid.
- Phototherapy, which involves exposing the skin to ultraviolet light on a regular basis under medical supervision. Tanning beds are not phototherapy.
- Traditional systemic treatments, taken by mouth, injection or infusion. These include acitretin, cyclosporine and methotrexate.
- Biologic agents, which are protein-based drugs that target specific parts of the immune system. These include traditional and recently developed versions of TNF-alpha blockers, as well as new classes of drugs, such as IL-17 inhibitors.
Early studies suggest that some new drugs might decrease the risk of co-morbidities associated with psoriasis—although more research is needed.
If you have psoriasis, you can take steps toward lessening your symptoms and safeguarding your overall health. They include:
- Seeking treatment for your psoriasis. Discuss treatment options with your dermatologist to decide together what is best for you. If you need help finding a dermatologist, the websites of both the American Academy of Dermatology and the National Psoriasis Foundation offer directories of physicians who are experienced in treating psoriasis.
- Seeing your primary care physician for regular checkups that include screening for other conditions that are more likely to develop if you have psoriasis. Early diagnosis can help limit the progression of serious illness.
- Relaxation. Stress can cause your psoriasis symptoms to flare-up, so find healthy ways to relieve your stress, from walking to yoga to relaxing with a good book.
- Following a healthy lifestyle. Eat a nutritious, balanced diet, stay active, limit alcohol and don't smoke.