Scientists identify marker for myeloid-derived suppressor cells
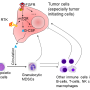
Myeloid-derived suppressor cells (MDSCs) are a population of immune cells that have been implicated in tumor resistance to various types of cancer treatment, including targeted therapies, chemotherapy and immunotherapy. Polymorphonuclear (PMN) cells represent the largest population of MDSCs. However, fully understanding the biology and clinical importance of these cells has been hampered by a lack of markers that set them apart from normal neutrophils.
Now, scientists at The Wistar Institute have identified a marker that distinguishes PMN-MDSCs from neutrophils in the blood of patients with a variety of cancers. Study results published in the journal Science Immunology also showed that higher numbers of cells positive for the marker were associated with larger tumor size.
"Before we started this work, the only way to isolate PMN-MDSCs was by density centrifugation of blood because they could not be properly identified in tumor tissue," said Dmitry I. Gabrilovich, M.D., Ph.D., Christopher M. Davis Professor and professor and program leader of the Translational Tumor Immunology program at Wistar, and senior author of the study. "Identifying a marker for PMN-MDSCs will allow us to study these cells in much more depth. In addition, if our clinical results are verified in larger studies, the marker could also be used to help physicians and patients make informed treatment decisions and, ultimately, it could be exploited to target PMN-MDSCs for therapeutic benefit."
MDSCs are potent suppressors of immune responses. They naturally regulate immune responses in healthy individuals, but the population rapidly expands in patients with cancer, and the presence of these cells has been associated with poor patient outcomes. One of the few ways to know for sure that cells are MDSCs is by showing that they suppress immune responses in vitro.
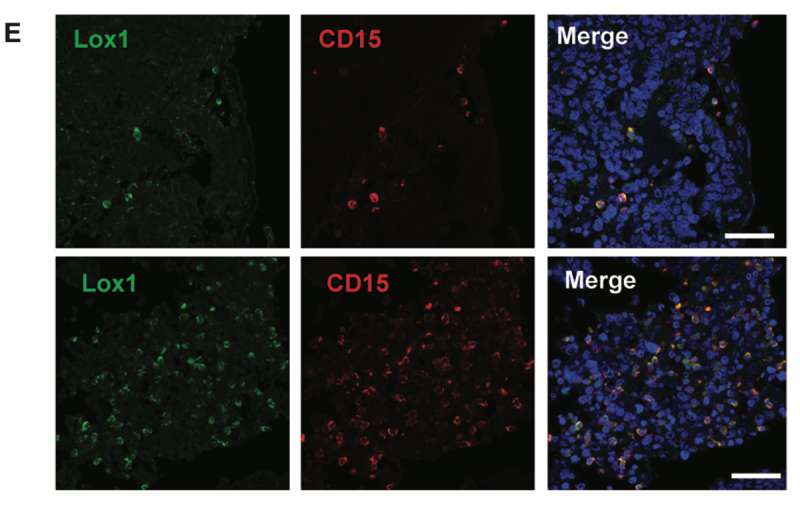
Gabrilovich and colleagues used whole-genome analysis to compare the genes expressed by PMN-MDSCs and neutrophils from the blood of patients with non-small cell lung cancer and head and neck cancer. The researchers focused on the genes expressed at higher levels in PMN-MDSCs compared with neutrophils, in particular those genes that encoded proteins detectable on the surface of cells. This led them to the protein LOX-1, which was almost undetectable on the surface of neutrophils but detectable on the surface of about one-third of PMN-MDSCs.
When they tested the ability of LOX-1-positive and LOX-1-negative cells to suppress immune responses in vitro only the LOX-1-positive cells had this function. The results showed that LOX-1 was a marker of PMN-MDSCs.
Gabrilovich and colleagues speculated that the number of LOX-1-positive PMN-MDSCs in blood and tumor samples from patients with cancer might help predict disease severity and outcome. They had samples from only a few patients with non-small cell lung cancer to study, but found that patients with larger tumors had higher numbers of these cells in both blood and tumor samples.
"Now that we have a specific marker for MDSCs, we can begin to ask new questions about the biology of these cells and their clinical significance," added Gabrilovich.
More information: Lectin-type oxidized LDL receptor 1 distinguishes population of human polymorphonuclear myeloid-derived suppressor cells in cancer patients, Science Immunology DOI: 10.1126/sciimmunol.aaf8943