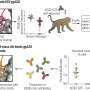
HIV expert's studies yielding insights into diseases of aging

While AIDS originally was seen as an adaptive immune disease, the research of Alan Landay, PhD, has contributed to a view of it as a cell driven-inflammation linked to immunosenescence—the gradual deterioration of the immune system that also accompanies normal aging.
Landay is professor and chair of Rush University's Department of Immunology and Microbiology and principal investigator of the National Institutes of Health-funded Rush Immunology Specialty Laboratory, or ISL. The lab is part of the NIH's AIDS Clinical Trials Group.
He has 35 years of experience in studies of HIV immunopathogenesis (the immune system response to HIV), has worked with the AIDS Clinical Trials Group since it was established in 1987 and has directed the ISL since it began. This research has resulted in Landay publishing more than 400 peer-reviewed papers that have helped shape current thinking about HIV and AIDS.
Here, he discusses how his HIV studies provide insight into common diseases of aging, including Alzheimer's disease.
Question: Why is the study of HIV so interesting to you?
Landay: Our study of HIV has given us important insight into other diseases and into aging and what we call "inflammaging" (low-level inflammation that often occurs in older adults). We are now seeing serious non-AIDS conditions such as cardiovascular, metabolic, neurocognitive and bone disease in HIV patients who also have persistent inflammation.
We are looking at how to measure that inflammation and understand how it contributes to these diseases of aging, which occur earlier in HIV patients than in the general population. We're seeing development of immune changes in HIV patients at around age 50 that we see in the general population at 65 or 70.
So HIV gives us a potential model of aging and especially of the immune system.
You are also interested in the human microbiome, the microorganisms in the body. How does that relate to your other work?
We are discovering a lot about the microbiome and its relationship to the immune system. Many groups are looking at how the bacteria, viruses and fungi that live in the gut may affect the immune system and infectious disease like HIV. Additionally, there are studies on gut/brain axis and how the microbiome may be involved in diseases like Parkinson's, depression, and autism.
In normal aging, the gut becomes leaky as its barrier function declines. As products from the gut leak out, inflammation can result, which can further accelerate aging.
We're studying how this inflammation contributes to diseases of aging and how it is perhaps accelerated in HIV patients. This inflammation can also contribute to serious non-AIDS events, and we are now exploring ways to modulate the microbiome to see if we can repair the barrier function of the gut.
I think that knowledge about the microbiome will have an impact in almost every disease area, including cancer and autoimmune, infectious, and neurological disease, as well as organ transplantation. All of these can be potentially affected by changes in the microbiome.
We are hoping that our study of the gut will reveal signatures of change in the microbiome that may predict development of these diseases. More importantly, we hope that we can use preventive measures to modify the microbiome. We have some clinical studies now with HIV patients where we are exploring whether probiotics (bacteria that can aid digestion) can move the microbiome back from dysbiosis (a microbial imbalance in the digestive system) to eubiosis (a healthy balance).
You're also looking at cytomegalovirus, better known as CMV, a virus that infects more than half of adults but usually doesn't cause symptoms. How is it relevant to HIV research?
Almost all HIV patients are co-infected with CMV, which is a virus that may cause some of the consequences of aging. When we look at people as they age, we see that more of the immune system is focused around the response to CMV.
In the aging population, CMV appears to be an important virus that is contributing to inflammaging and immune senescence. We think it also plays an important role in driving inflammatory responses in our HIV population.
We have been thinking about therapies to reduce CMV, which we think may reduce the consequences of aging and inflammation. We've also studied CMV in Alzheimer's and published results indicating that this might be an important virus in the brain and a co-factor to Alzheimer's development.
Tell us about the latest research at Rush.
We are tracking a group of HIV patients as they move along and grow older. Thirty years ago, when HIV first gained widespread awareness, patients typically died within a month or two of diagnosis.
Now they are typically living a healthy life to an age that is only a few years short of normal. But they are contracting these diseases of aging, which is what we are studying.
We are studying the microbiome as one of the possible contributors to this accelerated aging. There are collaborators around the world who are involved in this subject. I was involved in organizing an HIV and Microbiome meeting, held on the National Institutes of Health campus last year, that focused on enhancing our understanding of the role of the microbiome in HIV pathogenesis, prevention and therapy.
In Chicago, with our Patient-Centered Outcomes Research Initiative, we are starting to think about obtaining microbiome samples from a large population base in the Chicago metropolitan area to see what kinds of trends we see.
You work with groups and research cohorts all over the world. Can you talk a bit about that?
I work across the world to set up collaborative networks on understanding the role of HIV in aging. I work with a lot of large NIH-funded networks, one of which is called the AIDS Clinical Trial Group Network. It's the largest network of in the world of people involved with research on AIDS therapies and includes the U.S. as well as the developing and developed world.
I also work with another HIV-funded study that is investigating the progression of HIV disease in women. It is called the Women's Interagency HIV Cohort. Other working groups include a Canadian study of HIV in aging and HIV studies in the Netherlands, Ireland and Australia.
It sounds like aging is at the top of the pyramid of all that you are studying.
Yes, it is. I am trying to understand the basic elements of what we can do in terms of aging. What do we look at regarding nutrition and exercise? How can we apply the tools we have discovered to counter age-related diseases? I am working with colleagues to see how I can use my expertise in HIV and apply it to other important questions in the aging population.
As I said, people with HIV are living longer, and they are not dying of HIV but rather of other non-HIV diseases and co-morbidities—the same ones that are affecting the rest of the aging population. I think the fact that I was educated as a basic immunologist and also had clinical immunology training helps to break down some of the conceptual barriers.