Study adds to evidence listeriosis is unrelated to lowered immunity in pregnancy
A newly identified bacterial protein that is shown to jump-start infection may be the culprit in a foodborne disease that strikes pregnant women in disproportionately high numbers, leading to miscarriage and pre-term birth in most cases. This finding, by scientists at UCSF Benioff Children's Hospital San Francisco, runs counter to conventional wisdom that attributes susceptibility to the disease in pregnant women to their compromised immunity.
Listeriosis is caused by Listeria bacteria, which are ubiquitous in the environment and have been identified in contaminated cantaloupes and ice cream in recent outbreaks. Listeriosis is 20 times more common in pregnant women than in non-pregnant adults and occurs more frequently in those with lowered immunity, such as cancer and transplant patients, newborns and the elderly.
Pregnant women with listeriosis typically experience mild flu-like symptoms such as fever, fatigue and muscle aches. But infections can lead to miscarriage, stillbirth, premature delivery or life-threatening infections in newborns.
Earlier Work Unraveled Mystery of Placenta
In the study, which is available in the current online issue of Infection and Immunity and scheduled to be printed in June 2017, researchers headed by senior author Anna Bakardjiev, MD, looked at pregnant guinea pigs, because the placentas and responses to Listeria closely resemble their human counterparts.
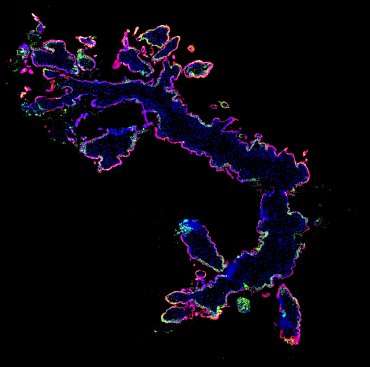
Previous research by Bakardjiev focused on unraveling a mystery: how bacteria invade the placenta, an organ that connects the uterus to the fetus and is normally responsible for providing a protective barrier against infectious agents. She found that a single bacterium was responsible for the infection that grew to very high numbers in the placenta, indicating another factor played a role in listeriosis.
"Given the unique immunological environment of the placenta, we hypothesized that virulence factors would be required for infection of this tissue that are not necessary for infection of other organs," said Bakardjiev, associate professor at UCSF Benioff Children's Hospital San Francisco in the Division of Infectious Diseases and the UCSF Microbial Pathogenesis and Host Defense Program.
In this current study, Bakardjiev and colleagues performed a genomic screen in pregnant guinea pigs that led to the identification of 201 Listeria genes implicated in infection of the placenta. Using genetic tools, they identified a protein secreted by Listeria that promotes placental infection, while having only a minor role in the infection of other organs.
'Virulence Factors' Required for Growth and Survival
In research with guinea pigs and mice, the scientists discovered that the protein, which they named InlP, increased the amount of bacteria in the placenta by 1,000-fold, while having minimal impact on other maternal organs.
"The findings challenge the dogma that pregnant women are susceptible to listeriosis because of immune compromise," Bakardjiev said. "Instead, placental pathogens need specific virulence factors that allow them to grow and survive in this niche.
"InlP presents a novel tool that we can use to better understand the course of placental infections, which is necessary for the development of new strategies to prevent and treat listeriosis and other infection-related pregnancy complications."
Listeria is the third leading cause of death from food poisoning in the United States, according to the U.S. Centers for Disease Control and Prevention. An estimated 1,600 people get sick from Listeria each year and one-third of these cases are associated with pregnancy. Approximately 260 people die from listeriosis.
More information: Cristina Faralla et al. InlP, a New Virulence Factor with Strong Placental Tropism, Infection and Immunity (2016). DOI: 10.1128/IAI.00625-16