Genetic defect found to cause disease in multiple organs
New research from Queen Mary University of London (QMUL) has identified a novel syndrome in patients with kidney and adrenal disease.
The research, published in the Journal of Clinical Investigation, identified defects in a novel gene called sphingosine-1-phosphate lyase (SGPL1) which causes multi organ disease particularly affecting the kidneys and adrenal glands. This may represent a novel lipid storage disorder similar to Niemann-Pick and Fabry disease, which are multi-systemic and progressive, often with neurological involvement.
The QMUL study involved patients from UK, Turkey, Pakistan, Spain and Peru and sequencing their DNA revealed the defective gene. Surprisingly, not all patients have the same symptoms, in some the kidney disease predominates and in others the adrenal dysfunction is the first symptom to emerge.
Lead researcher Dr Lou Metherell from QMUL's William Harvey Research Institute said: "The disease seems to be progressive, in some of our patients there has been a loss of motor and cognitive skills over time. Interestingly, the same gene defect has been linked to Charcot-Marie-Tooth neuropathy in another subset of patients.
"Getting a genetic diagnosis for these patients will allow for correct treatment, genetic counselling and careful monitoring to ensure any new symptoms are picked up early."
This study, which also involved QMUL researchers Rathi Prasad, Eirini Meimaridou, Helen Storr and Leo Guasti, highlights the importance of the sphingolipid pathway in adrenal and kidney function and suggests a potential role in other tissues such as the brain and thyroid.
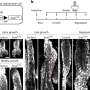
The team found the main characteristics of the human disease occurred in mice with the same genetic defect, and could provide a useful model to test treatments for this devastating disorder.
Since strategies to modify SGPL1 activity are being explored in the treatment of conditions such as multiple sclerosis and rheumatoid arthritis, understanding what happens when it goes wrong may provide important insights into the long-term effects of altering this pathway in patients.
More information: 'Sphingosine-1-phosphate lyase (SGPL1) mutations cause primary adrenal insufficiency and steroid resistant nephrotic syndrome' Journal of Clinical Investigation, jci.org/articles/view/90171