February 23, 2017 report
A possible way to detect the likelihood of infants developing type 1 diabetes later in life

(Medical Xpress)—A team of researchers with members from several institutions in Germany and one in the U.K. has discovered what might be a way to tell if a newborn child is likely to develop type 1 diabetes as they grow into teens. In their paper published in the journal Science Translational Medicine, the team describes a unique study they carried out involving at-risk children they had been studying since birth, and what they found with their T cells.
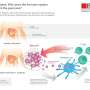
Type 1 diabetes occurs when the immune system, for unknown reasons, attacks and kills insulin-producing cells in the pancreas—this usually happens when people are in their teens. Prior research has shown that autoantibodies arise in children before diabetes symptoms occur, but there is little that can be done to stop the disease from progressing at that point. What scientists have been hoping to find is an indicator that shows itself long before the process is underway—perhaps during infancy. Such an indicator could offer help in two ways: first, by helping scientists to understand why the immune system goes rogue; second, by offering newly developed therapies an opportunity to do their work before the immune system activates.
In this new effort, the researchers have all been involved in diabetes research, and as part of that, have been collecting blood samples from some infants since 2000 that are deemed to be at high hereditary risk of developing diabetes. As those infants have matured into children, and some have developed the disease, the researchers have found themselves with an opportunity to compare immune development from birth between healthy children and those that developed diabetes. They found that when T cells in the infants that later developed diabetes came into contact with an antigen, some T cells were activated, which suggested they were already on the path to becoming autoreactive cells. This means that it might be possible to test all infants for a likelihood of developing diabetes simply by exposing a blood sample to an antigen to see if T cells become activated.
The researchers caution that their sample size was extremely small, so much more research needs to be done before developing a test can begin. In the meantime, the researchers and likely others will begin looking into why T cells in some infants appear to be so ready to be activated by an antigen.
More information: Anne-Kristin Heninger et al. A divergent population of autoantigen-responsive CD4T cells in infants prior to β cell autoimmunity, Science Translational Medicine (2017). DOI: 10.1126/scitranslmed.aaf8848
Abstract
Autoimmune diabetes is marked by sensitization to β cell self-antigens in childhood. We longitudinally followed at-risk children from infancy and performed single-cell gene expression in β cell antigen–responsive CD4+ T cells through pre- and established autoimmune phases. A striking divergence in the gene signature of β cell antigen–responsive naïve CD4+ T cells from children who developed β cell autoimmunity was found in infancy, well before the appearance of β cell antigen–specific memory T cells or autoantibodies. The signature resembled a pre–T helper 1 (TH1)/TH17/T follicular helper cell response with expression of CCR6, IL21, TBX21, TNF, RORC, EGR2, TGFB1, and ICOS, in the absence of FOXP3, IL17, and other cytokines. The cells transitioned to an IFNG-TH1 memory phenotype with the emergence of autoantibodies. We suggest that the divergent naïve T cell response is a consequence of genetic or environmental priming during unfavorable perinatal exposures and that the signature will guide future efforts to detect and prevent β cell autoimmunity.
© 2017 Medical Xpress