Highly effective cervical cancer screening for low income countries
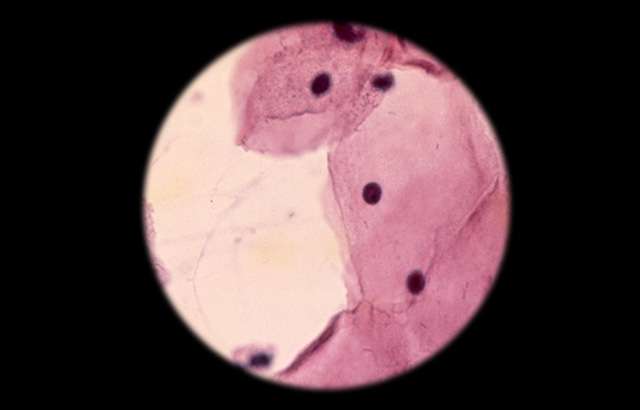
Cervical cancer is the second most common cancer in women in developing countries, and globally some quarter of a million women die from the disease each year - most of them from low and middle income countries (LMICs).
To reduce the incidence of cervical cancer in developed countries, nationwide screening is offered to all women. Taking a small cluster of cells ('cytology') to diagnose disease before it progresses to cancer has been extremely effective. But in less developed countries, a lack of infrastructure and quality management have hampered widespread implementation of effective screening programmes.
In the first study to evaluate the use of cytology to diagnose cervical cancer in LMICs, the researchers looked at cytology results from 717 cervical cancers from 23 studies in countries including India, Bangladesh, China, Thailand, Kenya, South Africa, Uganda, Peru, El Salvador, Costa Rica, Nicaragua, Brazil, Argentina and Egypt. They argued that cytology in these countries might be used to diagnose cervical cancer earlier.
An excellent screening tool
The researchers found that even in these low-resource settings, cytology was very sensitive and consistent for detecting invasive cancer. Cytology was found to successfully find cancer with 95.9 per cent accuracy in high-risk women showing symptoms.
Corresponding author Dr Alejandra Castanon from QMUL's Wolfson Institute of Preventive Medicine said: "Cytology has long been established as an excellent screening tool to prevent cervical cancer by detecting precancerous lesions. However, little research has been carried out regarding its sensitivity to cancer.
"We've found that this is an excellent tool for targeted screening of populations at high risk of cervical cancer, leading to early diagnosis. In resource-poor settings with limited facilities to treat advanced cancers, this could have a big impact on cervical cancer mortality."
Reducing burden and cost
The researchers say that restricting cytology to symptomatic women and referring only those with severe lesions would lead to substantially fewer women requiring further investigation. This could mean a reduction in burden on resource and cost, and could result in the diagnosis of cervical cancers at an earlier stage to improve overall survival from the disease.
Co-author Professor Peter Sasieni from QMUL's Wolfson Institute of Preventive Medicine added: "The implications are that, even when a country lacks infrastructure to implement a quality-assured cervical screening programme nationally, it might be able to facilitate early diagnosis of cervical cancer by using cervical cytology, and only referring women with severely abnormal smears."
The study was funded by Cancer Research UK and published in the Journal of Global Oncology.
More information: Alejandra Castanon et al. Systematic Review and Meta-Analysis of Individual Patient Data to Assess the Sensitivity of Cervical Cytology for Diagnosis of Cervical Cancer in Low- and Middle-Income Countries, Journal of Global Oncology (2017). DOI: 10.1200/JGO.2016.008011