Paradigm-changing clinical trial underway to better identify ureter during pelvic surgery
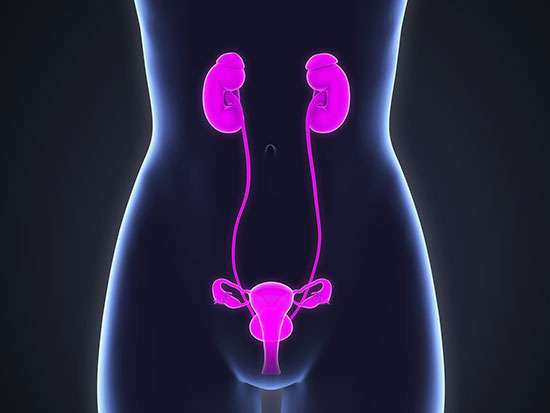
Women undergoing minimally invasive pelvic surgery are three to seven times more at risk of ureteral injury, the most common injury during this type of surgery. Warner K. Huh, M.D., director of the University of Alabama at Birmingham Division of Gynecology Oncology, is conducting a new clinical trial for an infrared imaging agent used in hysterectomy patients to better identify the location of the ureter—the passage between kidney and bladder—during surgery.
"Ureteral injury is perhaps the most feared injury for gynecologists," said Huh, the Margaret Cameron Spain Endowed Chair in the UAB Department of Obstetrics and Gynecology. "Identification laparoscopically can be challenging for gynecologists and colorectal surgeons, thus causing lots of guesswork."
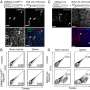
The study will use an investigational near-infrared contrast agent manufactured by LI-COR with the hope of identifying the ureter. Investigators will evaluate whether surgeons can visualize the ureter more clearly when the fluorescent contrast agent is administered at the time of surgery.
"If the contrast agent is proved safe and efficient in the clinical trial, this could shift the paradigm in gynecological surgery," Huh said. "Our number one priority is keeping our patients safe and performing surgeries to the best of our abilities."
More than 600,000 hysterectomy procedures are performed annually across the United States, with a marked rise in minimally invasive procedures and approaches, including robotic, laparoscopic and laparoscopic-assisted surgeries. In minimally invasive surgery, ureteral injuries are commonly due to inadvertent burning with electrocautery, the use of electricity to stop bleeding or cauterize blood vessels.
Seventy percent of injuries to the ureter are recognized postsurgery, and only 9 percent are recognized during surgery. Current strategies for identifying ureter injury during surgery include cystoscopy, a long viewing tube, a combination of cystoscopy and contrast X-rays to visualize the kidneys and ureters, or by passing a blue dye through the ureter to identify damage. Postoperatively, gynecologists can identify ureter injury via renal ultrasound, X-ray examination of the kidney, ureters and urinary bladder with iodine contrast, or CT imaging.
To repair the ureter, a second surgery or more may be required.
"Surgical morbidity to repair ureteral injuries is substantial," Huh said. "We hope that this new agent can help improve outcomes and reduce the risk of inadvertent injury overall for patients undergoing minimally invasive pelvic surgery."
LI-COR is involved in 15 clinical trials worldwide for intraoperative surgical solutions using its near-infrared dyes. This trial represents the first study that the company is directly sponsoring. If studies demonstrate the safety and efficacy of the near-infrared imaging agent, LI-COR plans to seek approval from the United States Food and Drug Administration and to commercially manufacture the product at its Lincoln, Nebraska, facility.