Brain microenvironment makes HER2-positive breast cancer metastases resistant to treatment
While target therapies directed toward genetic mutations that drive a tumor's growth have significantly improved the outlook for many patients, they have not been as successful in controlling brain metastases in several types of cancer. In the case of breast cancer driven by overexpression of the HER2 gene, up to 50 percent of patients treated with targeted therapies eventually develop brain metastases, which are inevitably fatal. Now a Massachusetts General Hospital (MGH)-based research team has identified a novel mechanism behind the resistance to HER2- or PI3K-targeted therapies and a treatment strategy that may overcome this resistance.
"While the failure of these drugs against brain metastasis has often been attributed to the blood brain barrier, some agents are small enough to penetrate into the brain," says Rakesh K. Jain, PhD, director of the Steele Laboratories of Tumor Biology in the MGH Radiation Oncology Department, co-senior author of the report published in Science Translational Medicine. "In addition, the disrupted, leaky vasculature that develops in and around tumors - what we call the blood tumor barrier - allows some accumulation of anti-HER2 and anti-PI3K drugs in brain metastases. This work shows that the tumor microenvironment itself can compromise the efficacy of targeted therapies and should be taken into account as new treatment approaches are developed."
The impact of the microenvironment on tumor growth and treatment has been a major focus of Jain's team. For this study they collaborated with Jeffrey A. Engelman, MD, PhD, co-senior author and a leading expert in targeted therapies, who was formerly with the MGH Cancer Center and is now Global Head of Oncology at the Novartis Institutes for BioMedical Research.
Co-first authors David P. Kodack, PhD, Vasileios Askoxylakis, MD, PhD, and Gino B. Ferraro, PhD - all of the Steele Labs - set out to identify factors in the brain microenvironment that could alter growth and survival signals within HER2-positive breast cancer cells. They and additional co-authors at the MGH Cancer Center, the University of North Carolina, Vanderbilt University and Novartis, identified HER3 - part of the same signaling pathway that includes HER2 - as a possible contributor to anti-HER2/PI3K resistance in breast cancer brain metastases.
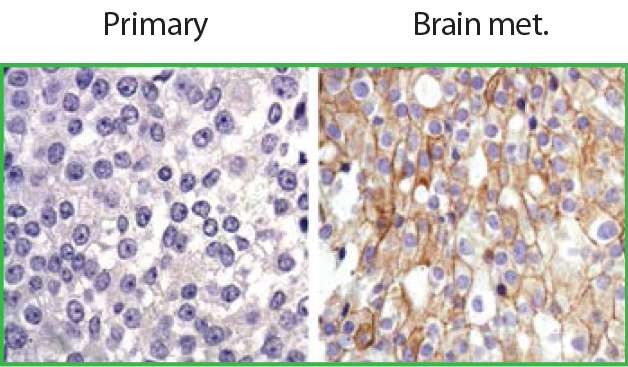
After confirming in mouse models that cells from HER2-positive breast cancers became resistant to anti-HER2 treatment when implanted into the brain but not into other tissues, the investigators found that HER3 is overexpressed in brain metastases of HER2- positive breast cancers from both mice and human patients. While neither a drug that targets HER3 nor one that interferes with the interaction between HER2 and HER3 were able to slow the growth of brain metastases, combined treatment with both an anti-HER2 and an anti-HER3 drug significantly slowed tumor growth.
"HER3 has been associated with treatment resistance in several types of cancer, and our findings indicate that the overexpression of HER3 within the microenvironment of brain metastases reprograms the signaling pathways shut down by HER2 suppression," says co-first author Ferraro. "We believe these findings will have a broad impact on the way targeted therapies are understood and applied. While therapies that target HER2 and HER3 are clinically available, clinical trials often exclude patients with brain metastases. These current findings must now be confirmed in patients for whom better treatment options are desperately needed."
More information: D.P. Kodack el al., "The brain microenvironment mediates resistance in luminal breast cancer to PI3K inhibition through HER3 activation," Science Translational Medicine (2017). stm.sciencemag.org/lookup/doi/ … scitranslmed.aal4682















