Bacteria from cystic fibrosis patient could help fight antibiotic-resistant TB
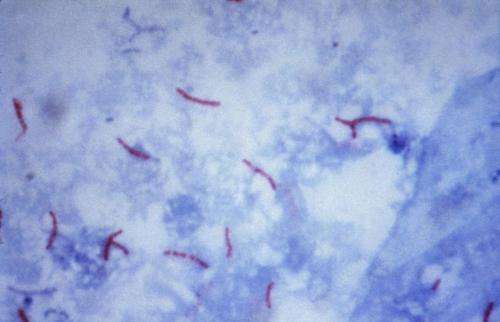
A newly discovered antibiotic, produced by bacteria from a cystic fibrosis patient, could be used to treat cases of drug-resistant tuberculosis (TB). This is the finding of a team of scientists from Cardiff University's School of Biosciences and the University of Warwick.
The problem of antibiotic-resistant infections is well documented, and it is estimated that by 2040, more than a third of all TB cases in Russia, for example, could show resistance to the drugs currently used to fight the disease. As pathogens continue to develop resistance to these once-reliable medicines, the search for new drugs has taken on a new urgency.
Among potential new drug sources is a group of the bacteria called Burkholderia that thrive in a wide range of natural habitats, but occasionally cause infection such as those within the lungs of people with cystic fibrosis. These microbes have adapted to these diverse environments in part by making potent antibiotics in order to take out their competition.
In light of the growing threat of drug-resistant pathogens, a team led by Professor Gregory L. Challis from the University of Warwick and Professor Eshwar Mahenthiralingam from Cardiff University set out to determine whether Burkholderia could potentially produce new antibiotics that could treat diseases such as drug-resistant TB. They were assisted by Professor Julian Parkhill (Wellcome Trust Sanger Institute, Cambridge, UK) and Professor Stewart Cole (Global Health Institute, Ecole Polytechnique Federale de Lausanne, Lausanne, Switzerland), who helped with DNA sequencing of the antibiotic producing bacterium and testing of tuberculosis, respectively.
The team discovered that one particular species, Burkholderia gladioli, which was isolated from the sputum of a child with cystic fibrosis, produces a new antibiotic they called gladiolin. This compound is similar in structure to another antibiotic that has been investigated for its ability to jam bacterial cell machinery, but gladiolin is much more stable and could therefore potentially be a better drug candidate. Further lab testing also showed that this antibiotic blocked the growth of four drug-resistant TB strains.
Commenting on the discovery, Professor Mahenthiralingam said: "This work is a continuation of our research on Burkholderia bacteria as a new source of antibiotics, and it has shown that Burkholderia gladioli, which we have historically studied as lung infections in people with cystic fibrosis, can also produce potent drugs for global infectious diseases such as antibiotic resistant tuberculosis.
"Having made this discovery we will now see if gladiolin can be taken forward as a potential drug for the clinic. Since this clinical testing process can take over a decade, it is vital we keep screening sources such as Burkholderia for other new antibiotics, and we hope that further research funding is made available to do this."
More information: Lijiang Song et al. Discovery and Biosynthesis of Gladiolin: A Burkholderia gladioli Antibiotic with Promising Activity against Mycobacterium tuberculosis, Journal of the American Chemical Society (2017). DOI: 10.1021/jacs.7b03382