New brain network model could explain differences in brain injuries
Considering the brain's network of activity, rather than just individual regions, could help us understand why some brain injuries are much worse than others, according to a study published PLOS Computational Biology by Maxwell B. Wang, Julia Owen, and Pratik Mukherjee from University of California, San Francisco, and Ashish Raj from Weill Cornell Medicine.
The human brain displays an astonishing range of responses to injury, depending on its location. This is conventionally considered a result of the fact that each brain region has a specific functional role. However, there is increasing evidence that the brain's regions do not operate in isolation but as a network or 'connectome.' Therefore, to understand the effect of injury, we must look not just for localized changes but network-wide changes caused by the disruption of network connections.
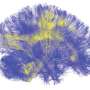
The authors used a combination of Diffusion-Tensor MRI and ideas from graph theory to investigate patterns in the white matter network architecture of the brain, and how these change due to injury. They built on previous work by Dr. Raj, in the Feil Family Brain and Mind Research Institute at Weill Cornell Medicine, and colleagues that showed that simple models of networks capture brain-wide patterns of degeneration as well as normal patterns of brain activity. These patterns can be decomposed into the network's "eigenmodes," which may be thought of as sub-networks into which reverberatory or propagating activity gets concentrated, not unlike vibrating modes on a guitar string.
The authors first showed that the most important eigenmodes are persistently found across healthy subjects, and in multiple scans of the same subject. They modelled the effect of brain lesions on eigenmodes and found that the influence of a lesion on network eigenmodes is fairly sensitive to the site of the lesion. The researchers identified white matter fiber pathways that were particularly responsible for the flow of information throughout the brain. They found that the lesions that most influenced network eigenmodes were those at the center of these pathways.
They looked in particular at a rare neurodevelopmental disorder where the corpus callosum, the primary connection between the left and right hemispheres of the brain, is absent. Patients suffering from this disease typically fare much better than those whose corpus callosum is surgically removed, an observation which can be explained using the eigenmode model.
If these findings can be replicated in other scenarios, it could be possible to predict with greater accuracy how future changes to brain structure, such as surgery or the progression of a disease, would result in changes to brain function, allowing physicians to better tailor treatment plans and therapeutic targets.
"This study proposes a method to relate how changes in the brain's structural architecture can result in the observable deficits we identify with neurological disorders. We hope to extend these methods towards predicting how future perturbations to a patient's brain, either from the progression of a disease or a novel therapeutic, can affect neurological function," says senior study author Dr. Raj.
More information: Wang MB, Owen JP, Mukherjee P, Raj A (2017) Brain network eigenmodes provide a robust and compact representation of the structural connectome in health and disease. PLoS Comput Biol 13(6): e1005550. doi.org/10.1371/journal.pcbi.1005550