Study links immune responses to intestinal microbes with rheumatoid arthritis
In patients with rheumatoid arthritis (RA), self-reactive T cell responses cause inflammation and progressive damage to synovial joints. Although genetic risk factors for RA have been identified, environmental causes are also thought to play a role in the onset of RA. Recent work suggests that the disease is initially triggered by immune responses to gut bacteria, but how autoimmunity of intestinal origin plays a role in RA-linked autoimmune responses is unclear.
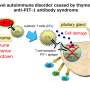
This week in the JCI a study led by Annalisa Pianta at Massachusetts General Hospital describes two proteins derived from common types of gut bacteria that evoke immune responses in RA patients. N-acetyl-glucosamine-6-sulfatase (GNS) and filamin A (FLNA) were identified as autoantigens that produce responses from both T and B cells in over 50% of RA patients, but not healthy controls or patients with other rheumatic diseases. Although GNS and FLNA antigens were discovered in the synovial joint fluid in RA-affected joints, GNS and FLNA proteins show remarkable similarity to proteins produced by common classes of intestinal bacteria.
It is still unclear how abnormal immune responses to gut bacteria develop and transition to autoimmune destruction of joints in RA patients. However, the findings of this study support the hypothesized link between intestinal and synovial autoimmunity. In addition, the specificity for GNS and FLNA autoantigens for RA provides a pathway for the development of approaches to improve diagnosis and treatment of this disease.
More information: Annalisa Pianta et al, Two rheumatoid arthritis–specific autoantigens correlate microbial immunity with autoimmune responses in joints, Journal of Clinical Investigation (2017). DOI: 10.1172/JCI93450