Research identifies how master regulator, bone-building protein can be used for therapy
The WNT1 ligand has previously been identified in bone disease, but its role in bone homeostasis, its cellular source and targets in bone have only just recently been identified. The research, led by Dr. Brendan Lee at Baylor College of Medicine, appears in the Journal of Clinical Investigation.
To determine the bone-specific function of WNT1, the mutation that has been associated with recessive forms of Osteogenesis Imperfecta (OI) and other forms of early-onset osteoporosis, Lee, chair of the Department of Molecular and Human Genetics at Baylor, generated mouse models to study the consequences of both the loss and gain of WNT1 function in a specialized bone cell called the osteocyte.
"This research builds on previous work that identified WNT1's role in coordination and its known effect on brain development. Now, we understand how this molecule works in bone, and this paper tells us that WNT1 is produced by osteocytes to control the activity of the bone-forming cell, the osteoblast," said Lee, also the Robert and Janice McNair Endowed Chair and professor of molecular and human genetics at Baylor.
The role of osteocytes, blasts and clasts
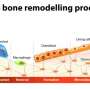
The over- or underexpression of WNT1 is controlled by osteocytes, or bone embedded cells. The osteocytes produce WNT1 to signal to bone-forming cells called osteoblasts that reside on the surface of bone via a biochemical pathway called mTORC1. When WNT1 is overexpressed by the osteocyte, bone formation is stimulated due to an increase in osteoblast numbers and collagen production following the activation of the mTORC1 pathway in these cells.
"Osteocytes are embedded in the bone, with osteoblasts and osteoclasts sitting on the surface adding or removing bone, respectively," explained Lee. "It turns out, osteocytes are actually the master controllers of this balance of bone formation and resorption in part by acting as either a receiver or sender of WNT signals."
"We knew previously from others' work that osteocytes could inhibit bone formation by producing the protein sclerostin, which represses osteoblast function. This research brings the cycle of information full circle by showing that while sclerostin turns the osteoblasts off, WNT1 from osteocytes turns them on," Lee said.
On the other hand, loss of WNT1 function resulted in low bone mass and spontaneous fracturing, similar to that seen in patients with OI. In this case, the osteocyte is not producing WNT1. However, osteocytes also can receive WNT signals themselves, leading them to control the activity of bone-removing cells, the osteoclasts.
Therapeutic impact
Primary therapies traditionally used to treat OI have shown limited efficacy in combating WNT1-related OI and osteoporosis. However, Lee and his research team identified anti-sclerostin antibody (Scl-Ab) treatment is effective in augmenting the action of other WNT ligands to improve bone mass and to significantly decrease the number of fractures in swaying mice, a model of WNT1 related OI and osteoporosis.
"The results of this study, while conducted in mice, have important implications for the treatment of OI and osteoporosis in humans down the road," Lee said. "By blocking sclerostin, the bone can be repaired effectively in diseases related to loss of WNT1 suggesting a personalized therapy. This is exciting especially as a promising anti-sclerostin drug is already in clinical development."
More information: Frank Rauch. The brains of the bones: how osteocytes use WNT1 to control bone formation, Journal of Clinical Investigation (2017). DOI: 10.1172/JCI95386