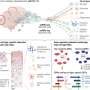
Study points to link between antidepressant use in pregnancy and autism in children

Children exposed to antidepressants during pregnancy seem to be at a slightly higher risk of autism than children of mothers with psychiatric disorders who were not treated with antidepressants during pregnancy, finds a study published in The BMJ today.
However, the researchers stress that the absolute risk of autism was small, so these results should not be considered alarming.
Depression is common in women of childbearing age, and in Europe 3-8% of pregnant women are prescribed antidepressants during pregnancy.
Several studies have reported associations between antidepressant use during pregnancy and autism in offspring. But it is not clear whether this is due to the underlying illness, antidepressant drugs, or other unmeasured factors.
Such factors (known as confounding) can introduce bias and affect the results of a study, making it difficult to draw firm conclusions about cause and effect.
In a bid to minimise the effects of confounding - and better understand the reasons behind this association - a research team led by Dheeraj Rai at the University of Bristol applied a range of analytical methods to a large Swedish population.
They analysed data from 254,610 individuals aged 4-17, including 5,378 with autism, living in Stockholm in 2001-11 who were born to mothers who did not take antidepressants and did not have any psychiatric disorder, mothers who took antidepressants during pregnancy, or mothers with psychiatric disorders who did not take antidepressants during pregnancy.
Of the 3,342 children exposed to antidepressants during pregnancy, 4.1% (136) had a diagnosis of autism compared with 2.9% (353) in 12,325 children not exposed to antidepressants whose mothers had a history of a psychiatric disorder.
There was no evidence of any increased risk of autism in children whose fathers were prescribed antidepressants during the mothers' pregnancy.
The results of the various analyses seemed to be consistent with each other, say the authors, suggesting that the association between antidepressant use in pregnancy and autism might not be fully explained by confounding.
They point to some study limitations, such as lack of detailed measures of severity of depression. However key strengths were the large sample size and the range of analyses carried out to minimise bias.
So what should families and doctors making decisions about antidepressants during pregnancy make of such results?
It is important to note that the absolute risk was small (over 95% of women in the study who took antidepressants during pregnancy did not have a child with autism), stress the authors.
They estimate that, even if the association between antidepressant use and autism is causal, only 2% of cases would be prevented if no women with psychiatric disorders used antidepressants during pregnancy.
They call for "a balanced discussion in relation to clinical decision making in the light of evolving but yet inconsistent evidence" and say "it is important to continue investigation of possible underlying biological mechanisms that could help us to better understand the aetiology of autism."
In a linked editorial, Diana Schendel at Aarhus University in Denmark says the findings of this study "should be viewed through the kaleidoscope of possible causes of autism" and calls for future studies to be better powered, and include measures of maternal disease severity, more reliable measures of antidepressant use, and, ideally genetic markers.
She points to the "reassuring study message" that more than 95% of women in the study who took antidepressants did not have a child with autism.
Although such a small risk within a population might seem too high from an individual's perspective, "it must be carefully weighed against the substantial health consequences associated with untreated depression," she concludes.
More information: BMJ (2017). www.bmj.com/content/358/bmj.j2811
BMJ (2017). www.bmj.com/content/358/bmj.j3388