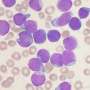
CLL evolution under the microscope
How do initially benign forms of cancer evolve to become aggressive? In a quest to answer this long-standing question, an EU project has studied the growth and clonal evolution of chronic lymphocytic leukaemia (CLL)—a blood and bone marrow cancer that mostly starts asymptomatic but can become very aggressive over time.
Cancer evolution is a complex process. Whilst we know that tumour growth is enabled by a continuous process of clonal expansion, genetic diversification and clonal selection, there are still many open questions related to this process. Answering them could be the key to preventing tumour progression and relapses.
According to Dr Michaela Gruber, whose research was funded under the CLL_INCLONEL (Identification and functional dissection of key genetic events in early chronic lymphocytic leukaemia) project, CLL is a valuable model for studying this process due to its high prevalence, initially slow progression and easy access to samples.
Dr Gruber studied the clonal dynamics of a cohort of 21 CLL patients, who were recurrently sampled from diagnosis until the time of first treatment. Her objectives were to identify events leading to disease progression using next-generation sequencing of patient samples. She also developed in vitro models to assess the functional impact of these genetic events on B cell biology, studied their impact on CLL and gathered valuable information on the effects of drugs on potential CLL sub-populations.
Dr Gruber agreed to discuss the project's outcomes and how they could one day lead to individualised diagnostic and therapeutic management of CLL.
What kind of knowledge did you aim to gather from this project?
The key aim of this project was to gain a better understanding of the early dynamics of growth and clonal evolution, as cancer progresses from diagnosis to the need for treatment. CLL is a highly informative model system for studying such natural cancer growth patterns: It typically has a relatively indolent beginning, with potentially long timeframes (in the order of years) before treatment becomes necessary.
Why is it so important to better understand clonal evolution? How can it help prevent tumour progression and relapse?
Insights from recent cancer sequencing studies indicate that the occurrence and expansion of cancer-driving mutations follows a specific sequence. Certain mutations generally appear to occur early in the disease and could be cancer-initiating. Other mutations tend to occur late and appear to have variable impact on tumour expansion. Moreover, different cancer sub-types show different patterns of mutations.
Together, these findings indicate that it could be possible to anticipate the specific evolutionary potential (i.e. plasticity) of a patient's cancer, which actually fuels progression, treatment resistance and relapse. Based on such understanding, therapeutic strategies could be shaped directly against this plasticity of cancer. This would be a major milestone towards overcoming current obstacles to cancer cure.
What would you say were the most important findings from the project?
Our data show that key mutations driving the progression of CLL are established very early in the course of the disease, years before symptoms warrant treatment initiation. For the first time, we were also able to quantify the impact of individual sub-clonal driver mutations on in vivo tumour expansion.
Another important discovery is that of clearly distinguishable growth patterns among patients, both globally as well as on a sub-clonal level. Finally, our data indicate that different patients have different potentials for clonal evolution and growth, and that these patterns remain throughout the entire course of the disease up to the event of relapse.
Can you tell us more about the genome editing technologies you employed?
Suitable experimental models are much needed in order to test the functional impact of observations made in CLL sequencing studies. Thus, we employed novel genome editing strategies, initially using TALENs and then switching to the recently emerged and more easily programmable CRISPR/Cas9 technology. Thanks to the latter, we established an array of isogenic B cell lines, which are used to test the molecular impact of mutations on cellular biology and—most important—treatment response.
What are your plans now that the project is completed?
We have initiated several follow-up projects in Vienna, which aim to integrate an understanding of epigenetic modifications and tumour microenvironments, as well as their role and dynamics in CLL evolution.
What do you hope will be the impact of the project on future diagnostics and treatments?
Our hope is to establish cancer evolution as a predictable process. With sufficient understanding of the forces that drive evolution and selective advantages of sub-clonal mutations, we hope to develop prognostic schemes that anticipate individuals' evolutionary trajectories.
Treatments based on these schemes would directly aim to target the cancer plasticity that underlies progression, treatment resistance or relapse. CLL provides us with a unique opportunity to better understand cancer evolution. The conceptual insights about cancer that can thus be gained from CLL would have a high potential for being translated across other haematologic and solid malignancies.
More information: Project page: cordis.europa.eu/project/rcn/186119