Could modifying gut microbes prevent or delay type 1 diabetes?
Autoimmune diseases such as type 1 diabetes are controlled by our genes. While researchers are eager to find out what other factors could contribute to this disease, a new study published by Yale researchers provides direct evidence that environmental factors, such as microbes that inhabit our intestines, may influence the incidence of the disease.
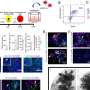
To probe the microbes-diabetes connection, the Yale team modified the gut microbiota of mice by co-housing non-obese diabetic mice with animals that harbored altered microbes. They found co-housed non-obese diabetic mice were less susceptible to diabetes. This co-housing led to an increased number of immune cells known as regulatory T cells in the gut, which likely contribute to this beneficial outcome, according to the researchers. By giving mice antibodies that have been used to treat diabetes in human clinical trials, they also observed that same type of regulatory T cells were increased. These T cells were mobile, allowing them to migrate to inflamed organs and suppress the other pathogenic T cells that cause the development of type 1 diabetes.
"The findings could lead to more effective strategies to prevent or treat type 1 diabetes and other autoimmune conditions by boosting protective T cells in gut-associated tissues," said Hua Yu, a postdoctoral fellow at Yale School of Medicine and first author of the paper.
Senior author and Sterling Professor of Immunobiology Richard Flavell added: "These strategies might include dietary, probiotic, or pharmaceutical approaches. For example, manipulating a patient's diet to enrich good bacteria and increase intestinal regulatory T cells might be critically important in type 1 diabetes management."
More information: Hua Yu et al. Intestinal type 1 regulatory T cells migrate to periphery to suppress diabetogenic T cells and prevent diabetes development, Proceedings of the National Academy of Sciences (2017). DOI: 10.1073/pnas.1705599114