An interdisciplinary approach to a better night's sleep

Most guidelines suggest adults get six to eight hours of sleep each night. Lichuan Ye, associate professor in the Bouvé College of Health Sciences, thinks about sleep for much longer than that each day. Indeed, her research focuses on promoting better sleep, and managing sleep disorders.
As a registered nurse and one of the Haley Nurse Scientists at Brigham and Women's Hospital, Ye, who joined Northeastern this fall, brings a unique perspective to the university and to her research.
"I have this mixed education and training background, so I love to explore the medicine of sleep, but I'm more behavior- and education-focused," she said. "That's how I started my clinical research."
That research, which has been published in the scholarly journal Sleep and covered by Reuters, examines the symptoms and treatment of sleep disorders. Most recently, she's focused on obstructive sleep apnea. The condition commonly leads to snoring and disrupted sleep, but can also cause sufferers to stop breathing altogether in more extreme cases.
However, the sleep apnea often takes a while to diagnose, Ye said. Her research includes examining how to better facilitate earlier diagnosis.
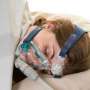
Treatment often includes wearing a continuous positive airway pressure, or CPAP, machine at night—a breathing mask that pushes a stream of air through the nose and mouth. But as Ye noted in her most recent publication on the topic, the biggest obstacle to treating obstructive sleep apnea is that people don't wear the mask. Or, if they do, they don't do it regularly.
So, her most recent research, supported by the National Institutes of Health, found that spouses play an important role in whether or not their partners do routinely use the CPAP machine.
Outside of those diagnosed with sleep apnea, there's another population that regularly grapples with disrupted sleep—hospital patients. Between the standard din of a busy hospital ward and the intermittent check of vital signs administered by hospital staff, it's hard for hospital patients to get more than a few hours of sleep at a time.
To address this issue, Ye helped develop the SLEEPkit, a sleep promotion toolkit for hospital staff. The kit, which is still being tested, will help hospital staff communicate with patients to gauge how to better enable uninterrupted sleep. For example, a stable patient may only need her vital signs checked every four hours instead of every two, Ye offered. Little changes like that could make a huge difference for the patient.
Ye, who helped create the very first sleep lab at the Hospital of the University of Pennsylvania, credits her interdisciplinary background for the way she approaches sleep—both as an academic and as a person deeply concerned with results.
"I love looking at patient outcomes, and interacting with real patients," she said. "That's where I feel like my studies can make a difference."
More information: L Ye et al. 0511 Spousal involvement in adherence to CPAP treatment, Sleep (2017). DOI: 10.1093/sleepj/zsx050.510