Serotonin promote liver regeneration following liver cancer treatment—but also supports early tumour regrowth
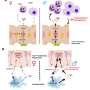
Blood platelets and serotonin – a molecule with growth promoting properties – stored in them play a significant role in the recurrence of cancer following partial hepatectomy. For the first time, a research group from MedUni Vienna has now proven these effects on tumour growth in humans. The results have recently been published in the Journal of Hepatology.
In a previous work dating from 2014, the group led by Patrick Starlinger from the Department of Surgery at Medical University of Vienna/Vienna General Hospital showed that high intra-platelet serotonin levels lead to a better clinical outcome following liver resection, since the serotonin stored in the platelets presumably has beneficial effects on post-operative liver regeneration, which subsequently might reduce the occurrence of complications. Based on this observation, it was hypothesised that influencing the serotonin level using drugs could boost liver regeneration and improve the outcome for patients following liver surgery. This concept would be very helpful in clinical routine, since approximately 10 – 20% of patients experience acute liver dysfunction following partial liver resection and there is currently no adequate treatment available.
Serotonin stimulates growth – both of the liver and the tumour
However, serotonin appears to be a relatively universal growth factor. Indeed, there are several scientific reports on the tumour-promoting effect of serotonin. In fact, numerous publications show that the main types of liver tumours display enhanced growth when stimulated with serotonin. However, there was only experimental data relating to this phenomenon and proof in the human system was still missing.
In order to evaluate the effect of serotonin on tumour growth in humans, patients undergoing liver resection were included in this study and serotonin levels in platelets were assessed before the operation. It has now been shown that patients with particularly low serotonin levels are more likely to suffer from complications and have a prolonged hospitalization after surgery than those with particularly high serotonin levels in their platelets.
However, if one looks at the recurrence rates for the resected tumours, the picture is very different: whereas patients with particularly high serotonin levels are more likely to experience early recurrence of cancer, those with very low serotonin levels are less likely to develop early tumor recurrence.
"The findings from this study are therefore of major importance for platelet-based treatment of post-operative liver failure," explains Patrick Starlinger, "While raising the amount of growth factors contained in the platelets, such as serotonin, has hitherto been regarded as an attractive treatment, we now see that this therapy also has a downside. Although higher serotonin levels reduce the risk of complications, in parallel, they increase the risk of developing early tumour recurrence within the first six months following liver resection with curative intent."
Serotonin was found to have this double-edged effect not only in primary liver tumours but also in metastases of colorectal cancer.
"These findings don't mean that platelet-based or serotonin-based treatment of post-operative liver failure should be abandoned completely" says Patrick Starlinger, clarifying the findings, "but rather the study shows that it is necessary to define the potential treatment very precisely and to evaluate the available options very carefully."
More information: Robin Padickakudy et al. Bivalent role of intra-platelet serotonin in liver regeneration and tumor recurrence in humans, Journal of Hepatology (2017). DOI: 10.1016/j.jhep.2017.08.009