Space station crew takes a breather with lung tissue investigation

The microgravity environment of the International Space Station impacts nearly every system within the human body. Researchers are studying the effects to the eyes, heart, muscles, and bones, but an area that hasn't received as much focus is one that is vital to human survival: the lungs.
Like a set of lungs, the Effect of Microgravity on Stem Cell Mediated Recellularization (Lung Tissue) investigation aboard the International Space Station is two-fold. First, researchers are studying the long-term effects microgravity may have on the lungs to gain insight into what countermeasures will need to be taken to protect crew members' lungs during long-duration missions. The investigation also will test strategies of lung recellurization, or the ability to grow cells into usable tissue on a natural lung scaffold, to be used for lung transplants on Earth.
Human lungs are sturdy and durable organs, but there isn't much definitive information regarding how they'll react during extended spaceflight. Every breath a person takes causes minor damage to their lungs. To battle this and maintain healthy function, lungs are constantly repairing and healing themselves. In microgravity, however, that process could change. The Microphysiological Human Organ Culture Model (MHOC), developed under a National Institute of Health grant, will tell researchers if our lungs stay just as strong and durable in space, or if they'll need extra help along the way.

"We need to understand how lungs heal over long-term spaceflight," said Joan Nichols, principal investigator for the investigation and professor of internal medicine, microbiology and immunology at the University of Texas Medical Branch. "If they don't heal properly, we might be able to come up with a microparticle therapeutic treatment that you breathe through an inhaler that would limit the damage that we're seeing or enhance the cells to do what you need them to do."
Part two of the investigation studies how microgravity may help to provide a more conducive environment for growing stems cells into lung tissue for transplants on Earth.
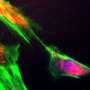
On Earth, stem cells attach to one another, divide a few times and mature into advanced tissue almost immediately afterward. In space, these stem cells have been known to stay pure and immature longer, a phenomenon Nichols calls "staying stemmy."
"It's hard, on Earth, for me to grow enough of these cells and expand them out because they start maturing immediately," said Nichols. "If I can grow more in space, then I might be able to take a sample, isolate those cells that I work with, grow them to high numbers and then come back and make a lung for replacement either using a whole natural lung scaffold or develop a bio printing technique to print one that fits perfectly."
Once the team grows enough of the stem cells, they are loaded on to a natural lung scaffold, a damaged, non-viable lung that has been drained of blood and cells, leaving only the structure of the organ. If research teams could grow enough cells on Earth, the stem cells use the scaffold to grow into a whole lung. Being able to grow these pure stem cells in microgravity and then bring them back to Earth for maturation on a scaffold could mean easier, more accessible lung transplants for patients who need them.
Tissue samples from the investigation were returned to Earth aboard the SpaceX Dragon spacecraft Sept. 17 and then to UTMB where they are undergoing analysis.