Mouse study adds to evidence linking gut bacteria and obesity

A new Johns Hopkins study of mice with the rodent equivalent of metabolic syndrome has added to evidence that the intestinal microbiome—a "garden" of bacterial, viral and fungal genes—plays a substantial role in the development of obesity and insulin resistance in mammals, including humans.
A report of the findings, published Jan. 24 in Mucosal Immunology, highlights the potential to prevent obesity and diabetes by manipulating levels and ratios of gut bacteria, and/or modifying the chemical and biological pathways for metabolism-activating genes.
"This study adds to our understanding of how bacteria may cause obesity, and we found particular types of bacteria in mice that were strongly linked to metabolic syndrome," says David Hackam, M.D., Ph.D., surgeon-in-chief and co-director of Johns Hopkins Children's Center and the study's senior author. "With this new knowledge we can look for ways to control the responsible bacteria or related genes and hopefully prevent obesity in children and adults."
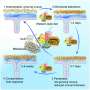
Metabolic syndrome, a cluster of conditions including obesity around the waist, high blood sugar and increased blood pressure, is a risk factor for heart disease, stroke and diabetes. While no precise cause for metabolic syndrome is known, previous studies of Toll-like receptor 4 (TLR4), a protein that receives chemical signals to activate inflammation, have suggested that TLR4 may be responsible in part for its development.
How and why TLR4 may be responsible for metabolic syndrome, however, has been unclear, says Hackam. Perhaps, the research team thought, TLR4 signaling in different cells and their association with the bacterial environment could result in different effects on the development of metabolic syndrome.
To first determine whether TLR4 specifically in the intestinal epithelium (layer of cells that line the small and large intestines) would cause the development of metabolic syndrome, the research team ran a series of experiments on both normal mice and mice genetically modified to lack TLR4 in their intestinal epithelium.
The researchers fed both groups of mice "standard chow," or food with 22 percent fat calories, for 21 weeks.
Compared to normal mice, those lacking TLR4 showed a series of symptoms consistent with metabolic syndrome, such as significant weight gain, increased body and liver fat, and insulin resistance.
The researchers then fed both groups of mice a high-fat diet comprised of 60 percent fat calories for 21 weeks to find out whether diet would affect the development of metabolic syndrome. Again, the genetically modified mice gained significantly more in weight and had greater body and liver fat than the normal mice.
To confirm the role of TLR4 expression in the intestinal epithelium, the researchers genetically modified three more groups of mice: one group expressed TLR4 only in the intestinal epithelium, another group lacked TLR4 in all body cells and the third group lacked TLR4 only in white blood cells.
All groups ate standard chow, and all groups had similar body weight, body and liver fat, and glucose tolerance compared to normal mice. Compared with normal mice, belly and small intestine fat was higher in mice lacking TLR4 only in the intestinal epithelium. This, the researchers say, provides further evidence that deleting TLR4 specifically from the intestinal epithelium is required for developing metabolic syndrome.
To investigate the role the bacterial makeup of the gut had on the mice, Hackam and his team then administered antibiotics to the normal and TLR4 intestinal epithelium-deficient mice. Antibiotics significantly reduced the amount of bacteria in the intestinal tract and prevented all symptoms of metabolic syndrome in the mice that lacked TLR4 in their intestinal epitheliums.
This demonstrates, the researchers say, that bacterial levels can be manipulated to prevent the development of metabolic syndrome.
To further explore the role of intestinal epithelial TLR4 on the development of metabolic syndrome, the research team analyzed fecal samples from the TLR4 intestinal epithelium-deficient and normal mice. The team found that specific clusters of bacteria that contribute to the development of metabolic syndrome were expressed differently in the deficient mice than in normal mice. They also determined that the bacteria expressed genes that made them "less hungry" and thus less able to digest the nutrients present in the mouse chow. This resulted in a greater abundance of food for the mouse to absorb, which contributed to obesity.
The researchers then analyzed the genes expressed in the lining of the intestinal mucosa—the site at which food absorption occurs—in normal and TLR4 intestinal epithelium-deficient mice. Of note, the team determined that important genes in the perixisome proliferator-activated receptor (PPAR) metabolic pathway were significantly suppressed in the deficient mice. Administering antibiotics prevented the differences in gene regulation between the two groups of mice, as did administering drugs to activate the PPAR signaling pathway, further explaining the reasons for which obesity developed.
"All of our experiments imply that the bacterial sensor TLR4 regulates both host and bacterial genes that play previously unrecognized roles in energy metabolism leading to the development of metabolic syndrome in mice," says Hackam.