Genetic factors driving natural variation in innate immune cell parameters

Why do people respond differently to infections or vaccines? Why are some people allergic to pollen? These are still unanswered questions in immune studies. A research consortium led by CNRS research director Dr. Lluis Quintana-Murci has recently described immune variation on a large scale within the French population. To achieve this, they studied an expansive collection of biological specimens from 1,000 French volunteers aged 20 to 69.
For many years, immunology focused on dissecting the molecular mechanisms that control physiological responses to infections based on the assumption that these responses do not differ among individuals. However, this premise has been challenged by recent studies suggesting that people are not all equally equipped to deal with pathogens. Age, sex, infection history, and genetics can affect the immune system and make people more prone to disease. The task of identifying these factors that regulate the immune system has become the main challenge facing precision medicine, a proposed medical model aimed at offering patient treatments tailored to individual needs.
Thus, some 30 scientists sought to describe immune variation on a large scale within the French population. This consortium gathered an expansive collection of biological specimens from 1,000 healthy donors (500 French men and 500 French women aged 20 to 69) recruited in Rennes. "The subjects' blood, DNA, vaccination and medical history, and intestinal and nasal bacteria were collected, measured and examined for this large-scale study," explains Lluis Quintana-Murci. The first results from analysis of the entire cohort were recently published in PNASand Nature Immunology.
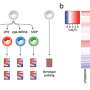
Using an ex vivo system, the researchers measured changes in immune gene expression in blood samples from the 1,000 donors when exposed to various viruses, bacteria, and fungi. At the same time, "we determined the molecular characteristics of the white blood cells, or leukocytes, in the donors' blood with an unprecedented level of precision," the CNRS researcher and study author Etienne Patin tells us. The two studies confirm that immune variation among individuals is largely due to differences in sex and age. "However, smoking and asymptomatic cytomegalovirus infection, which affects 35 percent of the population, also have a major impact on our blood cell composition. This may explain why smokers and people infected by this virus can be more prone to infection."
Genetic variations and risk of disease
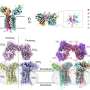
The researchers' next task was to determine whether our genetics contribute to immune response variation among individuals. "We identified hundreds of genetic variations that change the expression of molecules that play a key role in immune responses," says Lluis Quintana-Murci. "Some of them are associated with a higher risk of developing diseases such as pollen allergy, lupus erythematosus, and type 1 diabetes." These results shed new light on the potential causes of these illnesses, which remain unclear.
The Milieu Intérieur Laboratory of Excellence will now seek to determine whether intestinal and nasal flora and epigenetics (temporary changes in DNA) also contribute to immune variation. On a more general level, the extensive biobank developed for the purpose of this consortium will help identify disease risk factors, paving the way to precision medicine for infectious and autoimmune diseases.
More information: Natural variation in the parameters of innate immune cells is preferentially driven by genetic factors, Nature Immunology (2018). DOI: 10.1038/s41590-018-0049-7