HIV begins to yield secrets of how it hides in cells
UC San Francisco scientists have uncovered new mechanisms by which HIV hides in infected cells, resting in a latent state that evades the body's immune system and prevents antiviral drugs from flushing it out.
The findings, published online February 28, 2018, in Science Translational Medicine, could help scientists design and test new therapies aimed at curing a virus that still affects more than 1 million Americans.
Typically, HIV commandeers immune system cells called CD4 T cells and turns them into factories that can produce more virus. But for reasons that remain mysterious, a tiny fraction of these infected cells become dormant and do not make virus. Finding these "silent" HIV-infected cells is extremely challenging.
"We can't even separate out uninfected from infected cells, let alone latently infected cells," said Steven A. Yukl, MD, associate professor of medicine at UCSF and a staff physician at the San Francisco Veterans Affairs Medical Center. "Latently infected cells are extremely rare—one in 1 million CD4 T cells—and we don't know how to identify them."
Latently infected cells can remain dormant for decades—perhaps indefinitely—before encountering certain natural stimuli that cause them to start producing viral particles. Current antiretroviral therapies (ARTs) cannot kill latently infected cells, nor can they prevent them from reactivating. At best, ARTs can keep the virus at bay, but it usually rebounds as soon as patients stop taking the drugs.
"Knowing what mechanisms keep these latently infected cells silent would help us develop a therapy to either wake them up and kill them or silence them permanently," Yukl said. "Until we figure out what keeps them latent, we can't cure HIV."
Scientists at the UCSF-affiliated Gladstone Institutes had previously developed a device that could track HIV inside cloned laboratory CD4 cells, allowing them to scrutinize the entire course of an HIV infection, including the latency stage. But, since laboratory systems do not necessarily show what is really happening inside a human body, Yukl's team set out to examine cells taken from 18 HIV-infected patients.
Previously, researchers thought that latency stemmed from CD4 cells' inability to convert HIV DNA into viral RNA. It was thought that some unknown cellular mechanism was blocking the start of this DNA-to-RNA conversion process, called transcription, which meant that while the viral DNA persisted, it was never translated into viral proteins that would trigger a response from the body's immune system.
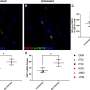
Yukl and his colleagues discovered that this wasn't the case. Using a panel of tests for different regions of the viral RNA (based on an amplification and quantification method called droplet digital PCR), the team detected multiple fragments of viral RNA, meaning that the process of converting the viral DNA to RNA was at least starting in latently infected cells.
These RNA fragments were almost all short or incomplete, however, which meant that the transcription process was stalling out at various stages. Infected cells were unable to make longer, full-length, or spliced viral RNAs, and the transcription process was never completed. These problems with transcription were reversed, however, when researchers activated the infected T cells.
"It's not that the cells aren't making viral RNA, but that the RNA isn't finished," Yukl said. To wake up latent cells, he added, the full viral transcription process needs to take place, and none of the currently available drugs can effectively complete this process. "Now we can start developing drugs that will make them finish the viral RNA, which can then be made into viral proteins so that the body can recognize and kill the infected cells."
Researchers have experimented with various 'latency-reversing' agents, although they are not yet used in the clinic. In the new study, the researchers discovered that each of these agents helped the cells at different steps along the process of making viral RNA, so a combination of them may be needed to completely activate the CD4 cells from their latent state.
"One of the nice things about knowing all these mechanisms is that we can look for new drugs or combinations and test how well they can overcome these transcription blocks," Yukl said. "It provides a roadmap to design and evaluate new therapies."
More information: Steven A. Yukl et al. HIV latency in isolated patient CD4 + T cells may be due to blocks in HIV transcriptional elongation, completion, and splicing, Science Translational Medicine (2018). DOI: 10.1126/scitranslmed.aap9927