Clinical trial tests tattoo sensor as needleless glucose monitor for diabetes patients

For Angela Valdez, being diagnosed with diabetes was an awakening. The disorder ran in her family, but she didn't think it would happen to her. And when it did, she acted by modifying her diet and physical activity. She was doing everything right—almost.
"I don't handle monitoring my diabetes as I should," said Valdez. "I have the diet down a lot better now and I take my medication as I should, but the finger pricking is a struggle for me. I only test if I feel bad. If I don't feel my blood sugar level is high, and I'm taking the pill every day, I think I'm alright. Which is really bad thinking, but the pin prick is terrifying."
Valdez one of 29 million people living with diabetes in the United States for whom monitoring their blood glucose (blood sugar) level is an integral component of managing their condition. Understanding how a patient's sugar levels ebb and flow over the course of time can guide medication regimens and suggest changes that may improve quality of life, perhaps even save it.
Unfortunately, like Valdez, many patients with diabetes do not track their blood glucose regularly. According to Edward Chao, DO, associate clinical professor of medicine at University of California San Diego School of Medicine and a physician at VA San Diego Healthcare System, one-quarter of persons receiving insulin treatment infrequently or never test their blood glucose. Another 65 percent of patients who use other drugs to treat their diabetes test just once a month or less.
"Adherence to chronic disease management is low—about 50 percent. Diabetes is no exception," said Chao. "There's more self-management involved in diabetes, including using needles to test blood glucose, monitoring foot health, managing medications and keeping regular clinical appointments. That's a lot more than many other conditions. We need to introduce a tool that reduces discomfort or inconvenience to increase vital monitoring of glucose."
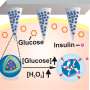
Enter a needleless glucose monitor dubbed the tattoo sensor, which measures insulin levels through sweat on the skin. Developed by UC San Diego Jacobs School of Engineering researchers and led by UC San Diego Center for Wearable Sensors director Joseph Wang, DSc, SAIC Endowed Chair of Engineering, and co-director, Patrick Mercier, PhD, the team is developing a glucose monitoring patch without the prick.
"Just like a kid's temporary tattoo, you apply it on the arm, dab with water and remove the back paper," said Mercier, an assistant professor in the Department of Electrical and Computer Engineering. "Our tattoo, however, is printed with material containing two electrodes that apply a small amount of electrical current. This forces glucose molecules that reside below the skin to rise to the surface, allowing us to measure blood sugar. It's safe and you can't really feel it."
Valdez has enrolled in a phase I clinical trial headed by Chao, in collaboration with Wang and Mercier. The ENGAGE study takes places at UC San Diego Altman Clinical and Translational Research Institute, where the team tests the tattoo sensor's accuracy at detecting glucose levels compared to a traditional glucometer.
Participants wear a sensor during fasting, at various times up to a couple of hours after eating. To validate accuracy, glucose levels from the sensor will be compared to results from simultaneous finger stick glucose readings.
"They placed the sensor on my shoulder and I washed it and dried it," said Valdez. "They said I should feel a mild sensation when they plugged in the electronic glucose monitor. I didn't. At one point it felt like a bug landed on me, but it was barely noticeable. After the first round I took a break to eat and work at my desk for a short time. I functioned like I normally do. I went back for the second round and didn't feel any discomfort. I can see wearing it all day."
The clinical trial is enrolling 50 adults, ages 18 to 75, with either type 1 or 2 diabetes or diabetes due to other causes. Type 2 diabetes occurs when the body cannot produce or becomes resistant to insulin—the master regulator of glucose storage and use. Type 1 diabetes is an autoimmune disease that destroys insulin-secreting beta cells in the pancreas, leaving the body unable to produce insulin.
By producing a noninvasive, discrete and user-friendly product that is inexpensive, the UC San Diego team hopes to break down barriers that deter patients from testing blood glucose regularly. If produced on a mass scale, Mercier believes the tattoos could be priced equally to what glucose test strips cost today, approximately $1 per single-use strip.
In its current stage, the tattoo sensor provides one readout. Eventually, Mercier hopes to have a continuous sensor that monitors glucose for a whole day.
Continuous glucose monitors already exist. However, the technology still requires inserting a needle into the abdomen every few days to measure glucose through interstitial fluid and requires calibrating with finger sticks periodically.
"Drawing blood is uncomfortable. No one likes doing it. The beauty of the technology we are developing is that it is a truly noninvasive means to measure glucose," said Mercier. "The main purpose of our research is to develop new technologies that can monitor glucose without drawing blood and ideally measure it over the course of the day. By giving this real-time information to patients, they can manage their consumption of sugars and injections of insulin much better than with periodic spot measurements."
Currently, to get the most up-to-date data, patients prick their fingers a few times per day. Blood is then applied to a glucose test strip which is inserted into a portable glucometer for analysis of glucose levels. The data gathered, however, is still limited. To get a better sense of a patient's overall health more frequent testing—or better yet, continuous monitoring—provides a fuller, more detailed picture of what is happening inside the patient's body when he or she eats or is active, said Chao.
"Even if you are not on insulin, it's useful to have a glucometer in times of rapidly changing glucose levels," said Chao. "We're not just trying to prevent dangerous highs and lows. That's the immediate feedback. In the long term, this allows us to discern patterns throughout the day when a person is running really high or having trouble spots when they're running hypoglycemic."
Hypoglycemia, or abnormally low blood sugar, can be dangerous and requires immediate treatment. A severe case might leave a person unable to treat themselves and could lead to seizures or even death. Diabetes is the seventh leading cause of death in the U.S.
Hyperglycemia or high glucose levels occurs when the body has too little insulin or isn't using insulin properly to moderate blood sugar. If untreated, hyperglycemia poses greater long-term consequences, including a condition called ketoacidosis or diabetic coma. Hyperglycemia can also increase a person's risk of diabetic complications, such as heart attack, stroke, peripheral atrial disease, blindness, kidney disease and more.
"There are times when people will notice that when their glucose is low. They may feel sweaty, shaky or irritable," said Chao. "But, some people may not recognize when they have hypoglycemia. People with high blood sugar may not feel any different and won't know they are running high. That's scary. That's where having a continuous glucose monitor will be very useful and lifesaving."