Punjab, India: Mass treatment of a population with chronic hepatitis C infection produces high rates of cure
A large-scale study evaluating the feasibility of decentralized care and the provision of free direct-acting antiviral agents (DAAs) has reported high rates of cure among a population of almost 20,000 individuals completing treatment for hepatitis C virus (HCV) infection. The study conducted in Punjab, India, which was reported today at The International Liver Congress 2018 in Paris, France, validated the efficacy and safety of generic all-oral DAA regimens delivered using a decentralized algorithm-based public health model.
'We have shown in our study that it is possible to cure more than 90% of individuals with HCV infection in a highly dispersed population using well-trained teams in government medical colleges and district hospitals, and widely available DAAs', said Professor Radha Krishan Dhiman from the Postgraduate Institute of Medical Education and Research, Chandigarh, India and lead author of the study. 'We believe the Punjab Model could be applied to many different populations with the aim of eliminating HCV'.
Hepatitis C virus (HCV) infection represents a major healthcare burden in India, with an estimated 12-18 million people infected. The burden is particularly heavy in the Indian state of Punjab, owing to the high prevalence of risk factors such as unsafe medical practices—including unsafe medical injections, blood transfusions and dental procedures—and intravenous drug use. Similar to other geographical regions in India, genotype 3 predominates in the state of Punjab.
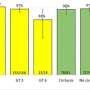
The study presented today by Prof. Dhiman formed part of a concerted effort in the Punjab region to both decrease the reservoir of HCV by treating established cases and reduce the incidence of new cases, and was made possible by the foundation in 2016 of the Mukh Mantri Punjab Hepatitis C Relief Fund, which provides free treatment to all individuals with chronic HCV infection. The study assessed the feasibility of delivering decentralized HCV care via three government medical colleges and 22 district hospitals, and required the training of approximately 90 medical specialists, pharmacists and data managers. Epidemiological data were managed with support from the Clinton Health Access Initiative. A cost-effective treatment algorithm was developed using sofosbuvir-based regimens to treat all patients with HCV infection, with regimens selected based on the presence/absence of cirrhosis and HCV genotype. A total of 29,371 patients (61.7% male; mean age 42 years) were enrolled in 1 year, of which 19,646 patients completed treatment with a sustained virological response (SVR) at 12 weeks of 92.5%. Cure rates among individuals with cirrhosis (93.1%) and without cirrhosis (92.4%), and those with genotype 3 (92.6%) and other genotypes (93.1%), were similar. No major adverse events were reported.
'This study is an impressive example of how to upscale the treatment of hepatitis C, which is important to reduce hepatitis C-related complications, particularly the development of hepatocellular carcinoma', said Prof. Markus Cornberg from the Hannover Medical School, Germany, and EASL Governing Board Member.