New tools could uncover important answers for Alzheimer's researchers
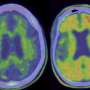
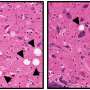
Alzheimer's disease currently affects more than 5.5 million Americans and is one of the costliest diseases to treat, according to the Alzheimer's Association. Characterized by a buildup of plaque in the brain, few animal models exist that researchers could use to study this devastating disorder. Now, a team of researchers from the University of Missouri, publishing in PLOS ONE, developed a rat model that can be used to study the buildup of amyloid plaques and vascular abnormalities in the brain.
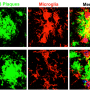
"One of the defining traits of Alzheimer's is the progressive accumulation of amyloid-β plaques in the brain," said Yuksel Agca, associate professor of veterinary pathology and a researcher in the Comparative Medicine Program in the MU College of Veterinary Medicine. "Two proteins, APP and PS1 are linked to the development of Alzheimer's disease in humans—and these two targets have become the basis for numerous studies. If we can identify how to manipulate amyloid-β build up, we can reduce the production of harmful plaques in the brain, leading to decreases in the onset of Alzheimer's disease."
The MU researchers developed rats that had human APP and PS1 proteins. The rats then underwent behavioral assessments in the Barnes maze. The maze, which tracks rodent behavior is used to measure learning and spatial memory. In a series of experiments, the Alzheimer's model rats that produced human APP and PS1 displayed poor memory and learning.
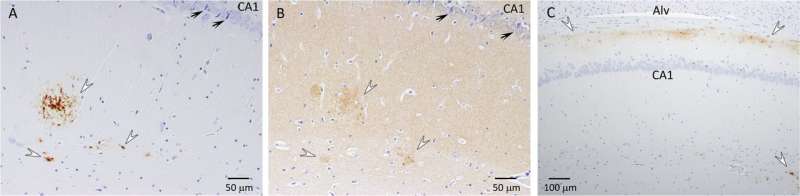
After the maze experiments, the research team assessed amyloid-β levels through serum tests, as well as brain screenings, which showed vascular changes and amyloid-β plaques similar to the ones observed in humans suffering from Alzheimer's disease.
"We found that these rat models could be useful in the fight against Alzheimer's in people," Agca said. "Because of their shorter lifespans and their larger size, translational models such as rats are extremely helpful in ongoing studies of disease. The results can be translatable to humans in identifying targets for drugs as well as identifying everyday lifestyle changes we can make to help stave off disorders like Alzheimer's. We hope this model will become beneficial as research continues to move forward."
Just like plaque on teeth or in arteries, plaque buildup in the brain can be decreased in people by maintaining a good diet and exercise, Agca said.
The study, "Memory deficiency, cerebral amyloid angiopathy, and amyloid-β plaques in APP+PS1 double transgenic rat model of Alzheimer's disease," was published in PLOS ONE.
More information: Diana Klakotskaia et al. Memory deficiency, cerebral amyloid angiopathy, and amyloid-β plaques in APP+PS1 double transgenic rat model of Alzheimer's disease, PLOS ONE (2018). DOI: 10.1371/journal.pone.0195469