Study challenges 'shock and kill' approach to eliminating HIV
Researchers have provided new insight into the cellular processes behind the 'shock and kill' approach to curing HIV, which they say challenges the effectiveness of the treatment.
Their study, published in the journal eLife, suggests the need to explore alternative treatment strategies against HIV—a virus which 36.7 million people globally were living with in 2016, with 1.8 million people becoming newly infected in the same year, according to figures from UNAIDS.
HIV is currently incurable, due to the persistence of latently infected cells—cells that host the dormant virus. The 'shock and kill' approach to treating the infection involves using latency-reversing agents (LRAs) to force the infected cells to produce HIV again (the 'shock' phase), while maintaining antiretroviral therapy (ART) to prevent the occurrence of new infections. This reactivation of HIV would cause the shocked cells to be killed directly or indirectly by ART (otherwise known as the 'kill' phase).
However, currently available LRAs have proven ineffective. A team of researchers from the Buck Institute for Research on Aging set out to understand why. "Several obstacles can explain the failure of LRAs, but the biggest challenge to date is our inability to accurately identify the number of cells in the HIV latent reservoir—the group of cells that are infected with HIV but do not produce new infections," says lead author Emilie Battivelli, Postdoctoral Research Scholar at the Buck Institute.
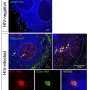
To address this challenge, Battivelli developed a new dual-fluorescence HIV-1 reporter virus, HIVGKO, to investigate the ability of various LRAs to reactivate HIV infection in latent cells. This virus encodes two different fluorescent proteins, GFP and mKO2. GFP is under the control of the HIV promoter and reveals the state of HIV transcription (latency versus productive), while mKO2 is under the control of a separate promoter (EF1alpha) and allows the identification of cells that are infected (latent and productive).
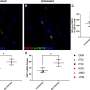
Using this reporter, the scientists discovered that a remarkably small number (less than 5%) of latently infected cells are reactivated by LRAs. Next, they carried out sequencing analysis of reactivatable versus non-reactivatable HIV infection in latent cell populations. This revealed that the sites where the virus integrates into the genome are distinguishable between viruses that reactivate and those that do not in response to LRAs.
"Together, these results indicate that while 'shock and kill' might be helpful in reactivating and possibly eliminating a small subset of highly reactivatable latent HIV genomes, other approaches will be necessary to control or eliminate the less readily reactivatable population identified both here and in patients," says senior author Eric Verdin, President and CEO of the Buck Institute.
"Perhaps this cell population should instead be 'blocked and locked' using latency-promoting agents, as previous research has suggested. For a functional cure, having non-reactivatable latent HIV genomes would surely be preferable to a lifetime of chronic active infection."
More information: Emilie Battivelli et al, Distinct chromatin functional states correlate with HIV latency reactivation in infected primary CD4+ T Cells, eLife (2018). DOI: 10.7554/eLife.34655