Cognitive training reduces depression, rebuilds injured brain structure and connectivity after traumatic brain injury
New research from the Center for BrainHealth at The University of Texas at Dallas shows that certain cognitive training exercises can help reduce depression and improve brain health in individuals years after they have suffered a traumatic brain injury (TBI).
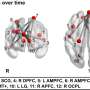
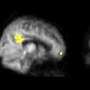
The recent study, published in Human Brain Mapping, revealed significant reductions in the severity of depressive symptoms, increased ability to regulate emotions, increases in cortical thickness and recovery from abnormal neural network connectivity after cognitive training.
"To our knowledge, this is the first study to report brain change associated with reduced depression symptoms after cognitive training," said Dr. Kihwan Han, a research scientist at the Center for BrainHealth who works in the lab of Dr. Daniel Krawczyk. Han is the lead author of the study.
"Overall, these findings suggest that cognitive training can reduce depressive symptoms in patients with traumatic brain injury even when the training does not directly target psychiatric symptoms," he said.
A past study involving the same protocol showed cognitive gains as well as similar changes in cortical thickness and neural network connectivity.
This study included 79 individuals with chronic TBI who all were at least six months post-injury. These individuals were randomly assigned into one of two groups: strategy-based training, which used the Strategic Memory Advanced Reasoning Training (SMART) program developed at the center; and information-based training, which used the Brain Health Workshop program. Researchers used the Beck Depressive Inventory to classify 53 of the participants as depressed.
The participants' depressive-symptom severity, psychological functioning scores and data from magnetic resonance imaging brain scans were collected before training, after training and three months post-training. Scans were used to study changes in brain structure and neural network connectivity.
Both training programs consisted of 12 one-and-a half-hour sessions over eight weeks that included quizzes, homework assignments, and projects conducted in small group settings that involved social interactions.
All participants in the depressed group showed significantly reduced depressive symptoms that were associated with improvements in cognitive and daily life functioning. According to Han, the social engagements, cognitive stimulation from new learning opportunities and hope of improvement afforded by both programs may help explain the reductions in depressive symptoms.
Based on the observed brain change patterns, Han suggested that improved emotion regulation also may be related to the reduced depressive symptoms. Over time, the reductions in depression symptom severity correlated with increased cortical thickness within the prefrontal cortex—an area of the brain responsible for executive functions needed for emotional control—and reductions in abnormally elevated neural connectivity within this region.
"Identifying what changes are happening in the brain when interventions successfully reduce depressive symptoms could allow us to create more effective, pharmaceutical-free approaches to help alleviate depression in people who experience chronic traumatic brain injury symptoms," said study author Dr. Sandra Bond Chapman, founder and chief director of the Center for BrainHealth, and Dee Wyly Distinguished University Professor.
More information: Kihwan Han et al. Neural correlates of reduced depressive symptoms following cognitive training for chronic traumatic brain injury, Human Brain Mapping (2018). DOI: 10.1002/hbm.24052