New device could mean end of the jab for people living with diabetes
Researchers from The University of Western Australia are testing the effectiveness of a device in the long-term treatment of the low blood glucose form of diabetes and are in need of community participants for the study.
Low blood glucose is a potentially fatal complication of diabetes, especially for patients who are on insulin. It effects many Australians every year and can result in seizures and nerve damage.
The Freestyle Libre Flash Glucose Monitoring System device is being tested in a study comparing usual care to the device lead by UWA researcher Professor Tim Davis and Research Nurse Penny Dwyer.
The trial could potentially lead to the replacement of the finger prick test and will make it much easier for patients to regularly monitor their blood sugar levels.
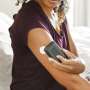
Research Nurse Penny Dwyer said the device comprises of a small disc with a fine needle that is inserted into the upper arm and connects to a blue tooth reader which allows glucose levels to be monitored in real time, at any moment throughout the day.
"It works by providing fast flow of readings throughout the day, so that if the blood sugar levels become too low the patient is quickly alerted and can take the steps to treat themselves," Ms Dwyer said.
"To complete the study we are in need of people who are over the age of 18 and who currently have had very low blood sugar level confirmed by a blood glucose machine of less than 4mmol/l."
Although the device is currently on the market, this is the first study to test its effectiveness against usual care in the long-term management of low blood sugar.
"We need to ensure that if people have a severe episode of low blood glucose they are prevented from having further episodes," Ms Dwyer said. "And this device looks like a good way of helping to prevent low blood glucose happening again."
Study participant Skye Windebank, 40, said she was first diagnosed with type 1 diabetes when she was 30.
"I've had four children including a twin pregnancy during that time which does a lot to your blood sugar levels," Ms Windebank said.
"The old way was to prick your finger and wait for the reading. so to do a test was a much more time consuming process and more of a hassle, especially with four young children and no routine. Using this new device is more convenient and I've been able to keep track of my blood sugar levels more frequently."
The researchers hope their trial will highlight the effectiveness of the device and could be used to make the device more accessible for people living with diabetes.
"This is a game changer. It means that in the future we may be able to get this device subsidised to help those living with diabetes, as it currently costs around $200 a month to use," Ms Dwyer said.