New study shows how gut immune cells are kept in control
Every day, the human gut works on a fine-tuned balance that ensures the retention of essential nutrients while preventing infection by potential armful microbes. Contributing to this surveillance system is a specialised group of immune cells that are held back due to unknown reasons, although they have many characteristics of activated cells. Now, a new study led by Marc Veldhoen, group leader at Instituto de Medicina Molecular João Lobo Antunes (iMM; Portugal) shows how these cells are kept under control. The work published now in Science Immunology reveals that the mitochondria of these cells have a different composition that reduces their energy production capacity, keeping them in a controlled activated mode. This knowledge can give rise to new diagnostics and treatments for conditions affecting the digestive tract such as gut inflammation or infections.
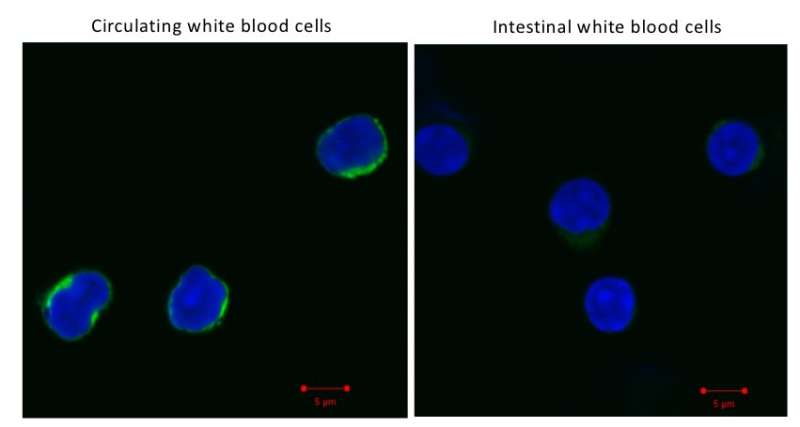
The skin and intestines contain a special population of white blood cells called intraepithelial lymphocytes. It has been largely unknown how the activity of these cells is controlled in a state that is neither fully activated nor at rest. Using imaging and biochemical experiments, the research group led by Marc Veldhoen has now shown this is partly due to differences in the cells' mitochondria. These energy-producing structures are present insideall cells. "We hypothesised that these gut-resident white blood cells may use energy in a different way. It was surprising to see that the detection of mitochondria gave a very different picture than seen in other white blood cells, forming the basis of a new hypothesis that the mitochondria themselves are different in these cells," explains Marc Veldhoen.
Using high magnification electron microscopy, the researchers observed that the mitochondria were present in abundance but seem to be different upon staining for light microscopy. Next, they studied the functionality of the mitochondria. "When we analysed these structures in detail, we found changes in the lipids that form a layer separating the mitochondria from the rest of the cell," says S?pela Konjar, joint first author of the study, adding that "these changes make the "batteries" work differently, as if they are in a "low energy mode."
When the lipid landscape was purposely altered, the researchers confirmed a change in the activation potential of the cells. "Our results showed that lipids in the mitochondria of these cells could alter their metabolic state and change their activity. When the mitochondrial lipids could not be arranged similarly to those found in other white blood cells, the cells could not be properly activated when needed," explains Marc Veldhoen. The researcher further explains: "This knowledge allows us to investigate how we can inhibit these cells when they are too active and cause damage, such as in gut inflammations, or how we can activate them more in cases of gut infections. Furthermore, the detection of mitochondria could be a diagnostic marker for the activation state of intestinal white blood cells."
More information: Konjar, S., Frising, U.C., Ferreira, C., Hinterleitner, R., Mayassi, T., Zhang, Q., Blankenhaus, B., Haberman, N., Loo, Y., Guedes, J., Baptista, M., Innocentin, S., Stange, J., Strathdee, D., Jabri, B., Veldhoen, M. (2018) Mitochondria maintain controlled activation state of epithelial-resident T lymphocytes. Sci. Immunol. 3, eaan2543. doi - 10.1126/sciimmunol.aan2543