Threat of malaria left its mark on the immune system in people with African ancestry
In a new study published June 7th, 2018 in PLOS Genetics, Christine Ambrosone of Roswell Park Comprehensive Cancer Center and colleagues identified a genetic difference between people with African and European ancestry that affects how the immune system triggers inflammation. They suspect these differences are rooted in how the immune system evolved and the evolutionary pressure exerted by malaria on ancestors who lived in Africa.
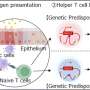
For thousands of years, the human immune system evolved to fight off constant assaults from a variety of infections, tailoring its response to defend against local threats. Thanks to modern hygiene, the immune system now faces far fewer attacks, but ancestral differences still remain, as demonstrated by differing disease rates between populations. To gain a better understanding of how different populations' immune systems respond to current lifestyles, researchers combined genetic, molecular and epidemiological data from in 914 people with African ancestry and 855 people with European ancestry from the African American Breast Cancer Epidemiology and Risk (AMBER) Consortium. They analyzed blood samples to detect 14 different chemical messengers involved in inflammation and identified significant differences between the populations in seven of those chemicals. Lifestyle factors such as age, education level, obesity, smoking and alcohol use could account for many of the differences, but the researchers also identified a genetic variant that occurred primarily in people with African ancestry. The variant controlled the levels of two key chemical messengers involved in recruiting white blood cells to sites of inflammation, and previous studies suggest it evolved to protect African individuals from contracting malaria.
The immune differences between people with European and African ancestry may have important implications for health that deserve further study. Inflammation has evolved as a response to injury and infection but is also implicated in several types of cancer and chronic disease. Ancestral "footprints" in the genome, such as the one identified in the study, may be exacerbating the health disparities observed between these two groups.
Corresponding author Christine Ambrosone adds: "We conducted this research based upon the hypothesis that adaptation over millennia to protect from infectious diseases in Africa, resulting in more robust immune response, could be related to more aggressive breast cancer in a modern environment. When we compared levels of certain inflammatory markers between women of African and European descent, we noted many differences. After we ruled out the effects of lifestyle factors, we found that much of these differences could be tied to the Duffy antigen receptor, whereby African Americans have a genotype that helps to protect from malaria."
"These findings indicate that evolutionary adaptation many thousands of years ago shaped our immune systems, and may still have considerable influences on immune function today", explains first author Dr. Song Yao. "The next research question we are pursuing is whether those evolutionary marks play any significant role in affecting breast cancer health disparities".
More information: Yao S, Hong C-C, Ruiz-Narváez EA, Evans SS, Zhu Q, Schaefer BA, et al. (2018) Genetic ancestry and population differences in levels of inflammatory cytokines in women: Role for evolutionary selection and environmental factors. PLoS Genet 14(6): e1007368. doi.org/10.1371/journal.pgen.1007368