A molecular key for delaying the progression of multiple sclerosis is found

Multiple sclerosis (MS) is an autoimmune disease that attacks and destroys the myelin sheath that insulates nerve cells. Current treatment is based on modulating the activity of the immune system or preventing immune cells from accessing the central nervous system and damaging it. These therapies are effective in the early phases of the disease, but they do not prevent its advance and the associated progressive functional deterioration.
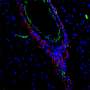
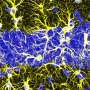
During the progressive phase of the disease, the microglial cells in the brain are the main cause of the chronic inflammation responsible for neurological deterioration. These microglial cells are the brain's sentries, reacting when faced with damage or infection. This reaction, which is in principle beneficial, becomes harmful when it is prolonged over time, leading to chronic inflammation, aggravating the disease and encouraging its progression.
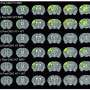
In the work just published, it was possible to identify a receptor known as P2X4 present in the microglial cells that increases their anti-inflammatory potential in order to reduce the damage in multiple sclerosis and encourage the body's own repair responses. This experimental development was conducted using animal models of MS, thanks to which it was possible to discover that the drugs that activate this receptor improve the symptoms during the chronic phase of the disease when furthering the repair of the nervous tissue.
Dr. María Domercq of the UPV/EHU's Department of Neurosciences and who works at the ACHUCARRO centre for research in Leioa (Basque Country) says, "We are witnessing a discovery that is opening up a new channel of pharmacological development for the treatment of the progressive phase of multiple sclerosis, and with it we want to open a new door on improving the life quality of people who suffer multiple sclerosis."
More information: Alazne Zabala et al, P2X4 receptor controls microglia activation and favors remyelination in autoimmune encephalitis, EMBO Molecular Medicine (2018). DOI: 10.15252/emmm.201708743