Study links aortic stiffness with lower cerebral blood flow
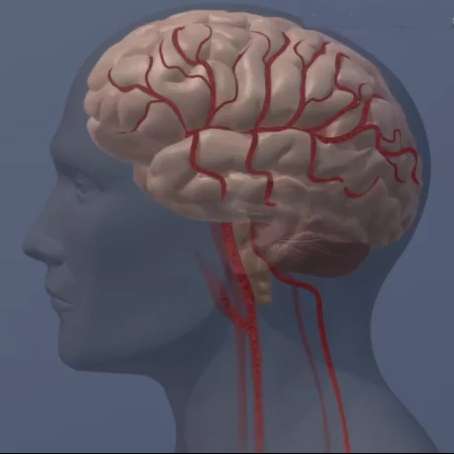
Greater aortic stiffness is related to lower cerebral blood flow, especially among individuals with increased genetic predisposition to Alzheimer's disease, according to research from Vanderbilt University Medical Center.
The study, published recently in Circulation, supports emerging evidence that arterial stiffness, a hypertension-related factor, may play a role in cognitive decline, said Angela Jefferson, Ph.D., professor of Neurology and director of the Vanderbilt Memory and Alzheimer's Center.
The study, which was conducted in older adults, showed a pronounced effect in the cognitively normal participants who carried the APOE4 gene, a susceptibility risk factor for Alzheimer's disease. It coincides with evidence announced in July at the Alzheimer's Association International Conference in Chicago that suggested intensive lowering of blood pressure in aging adults reduces the risk of mild cognitive impairment and may have implications for the prevention of Alzheimer's disease and dementia.
"Given our study results and the recent SPRINT MIND findings, we have to strongly consider whether more aggressive medical management of vascular risk factors, and hypertension in particular, can result in better late-life cognitive outcomes for aging adults," Jefferson said. "Collectively, results suggest that the answer is yes."
She and colleagues at Vanderbilt used cardiac magnetic resonance imaging to assess aortic stiffness across the aortic arch. The aorta, the largest artery in the body, is a compliant and flexible artery that naturally stiffens with age.
"The aorta constricts and dilates more than 40 million times per year," said Jefferson, the lead author of the study. "This amount of mechanical activity was perfectly fine back when life expectancy was 35 years of age, but life expectancy has more than doubled over the last couple of centuries.
"The aorta cannot withstand the excessive mechanical stress associated with so many additional years of constricting and dilating. As a result, the extracellular matrix within the vessel wall breaks down, and the aorta becomes increasingly stiff with age.
"It transitions from a flexible tube, like a garden hose, to something far stiffer, like a lead or concrete pipe," Jefferson said.
The study's findings add to a growing body of research detailing the strong connection between cardiovascular function and brain health as people age. A better understanding of this connection may lead to earlier detection and targeted interventions to prevent or mitigate consequences associated with aortic stiffening, including downstream cerebrovascular damage and further increases in blood pressure.
The research involved 270 participants in the Vanderbilt Memory and Aging Project, an ongoing interdisciplinary, longitudinal study being carried out at the Vanderbilt Memory and Alzheimer's Center. In addition to cardiac magnetic resonance imaging, participants also underwent brain magnetic resonance imaging.
"We examined blood flow in the brain using a sophisticated neuroimaging technique," Jefferson said. "Plus, we included a reactivity condition in which participants wear a mask that delivers just enough carbon dioxide to assess how responsive the cerebral vasculature is to subtle changes in arterial gas concentrations. If the vessels are healthy, they should dilate or expand to deliver more blood and oxygen to the brain."
Participants with the APOE4 gene had a more pronounced association between greater stiffness and lower cerebral blood flow, which was greatest in the temporal region of the brain.
"While there was an association between higher aortic stiffness, measured by pulse wave velocity, and reduced blood flow throughout the brain, what was particularly interesting is the interaction we discovered with the APOE4 gene," Jefferson said.
"Higher aortic stiffness related to lower cerebral blood flow in the temporal lobes, reflecting brain regions where Alzheimer's disease pathology first evolves. It is interesting that this Alzheimer's genetic risk factor modified the association in that way."