Biochemists described a new mechanism for autoimmunity suppression
RUDN biochemists suggested a new mechanism by which the human body prevents the development of autoimmune diseases, allergies and implant rejection. They report that regulatory T-cells are able to suppress the reproduction of autoimmune cells. The work was published in Molecular Immunology.
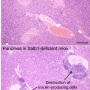
The ability of the body to resist pathogenic factors is under the control of immune cells, the most important of which are lymphocytes. The first subtype, called effector lymphocytes, contact with viruses and bacteria or cells affected by them, and kill the pathogens. After the pathogens are destroyed, such lymphocytes should die as well, otherwise they turn into autoimmune cells, causing autoimmune diseases and allergies by attacking normal cells. Another subtype, regulatory T-cells, prevents the development of such aggressive autoimmune cells. Scientists are aware that regulatory T-cells are able to suppress effector lymphocytes upon direct contact by activating special receptors on their membranes. Regulatory T-cells contact with the surface of the target cell and activate self-destruction processes.
"The mechanisms of autoimmunity suppression by regulatory T-cells are widely studied. However, it is not always obvious how they manage to react over distance. In our work, we've described a completely new distant (contact independent) mechanism based on "accelerated aging" of effector lymphocytes," says Dmitry Zhdanov, assistant professor of the department of biochemistry named after Academician T.T. Berezov at RUDN Institute of Medicine.
Each cell has a limited number of divisions. The regulatory mechanism for this limitation is quite simple and determined by nature itself. Upon each new division, the end regions of chromosomes, called telomeres, are reduced. After a certain number of divisions, the telomeres become critically short and the cells become aged (they are still alive but unable to divide). Afterward, these cells die. Unlike the majority of other cells, immune cells have an enzyme called telomerase that synthesizes telomeres. This allows lymphocytes to have more division instances and quickly reproduce in the event of an infection.
RUDN biochemists co-cultivated effector autoimmune lymphocytes and regulatory T-cells separated with a special membrane in one culture flask. The cells were unable to contact directly, but could distantly exchange soluble substances. It turned out that regulatory T-cells were able to inhibit the activity of telomerase in effector lymphocytes. Long-term cultivation of autoimmune lymphocytes with inactive telomerase caused their telomere loss and cell death. The effect was observed not only in the artificial conditions of cell co-cultivation, but also in living mice.
"Based on the obtained results we've described a new, previously unknown mechanism of autoimmunity regulation based on physiological aging of immune cells and the activation of their self-destruction processes. Obviously, this process is fundamental to support cell functions and determine the fate of the cells. The understanding of this mechanism may be useful for the development of treatments for autoimmune diseases and prevention of implant rejection," concludes Dmitry Zhdanov.
More information: Dmitry D. Zhdanov et al, Contact-independent suppressive activity of regulatory T cells is associated with telomerase inhibition, telomere shortening and target lymphocyte apoptosis, Molecular Immunology (2018). DOI: 10.1016/j.molimm.2018.07.017